What you need to know about Sclerotherapy procedure
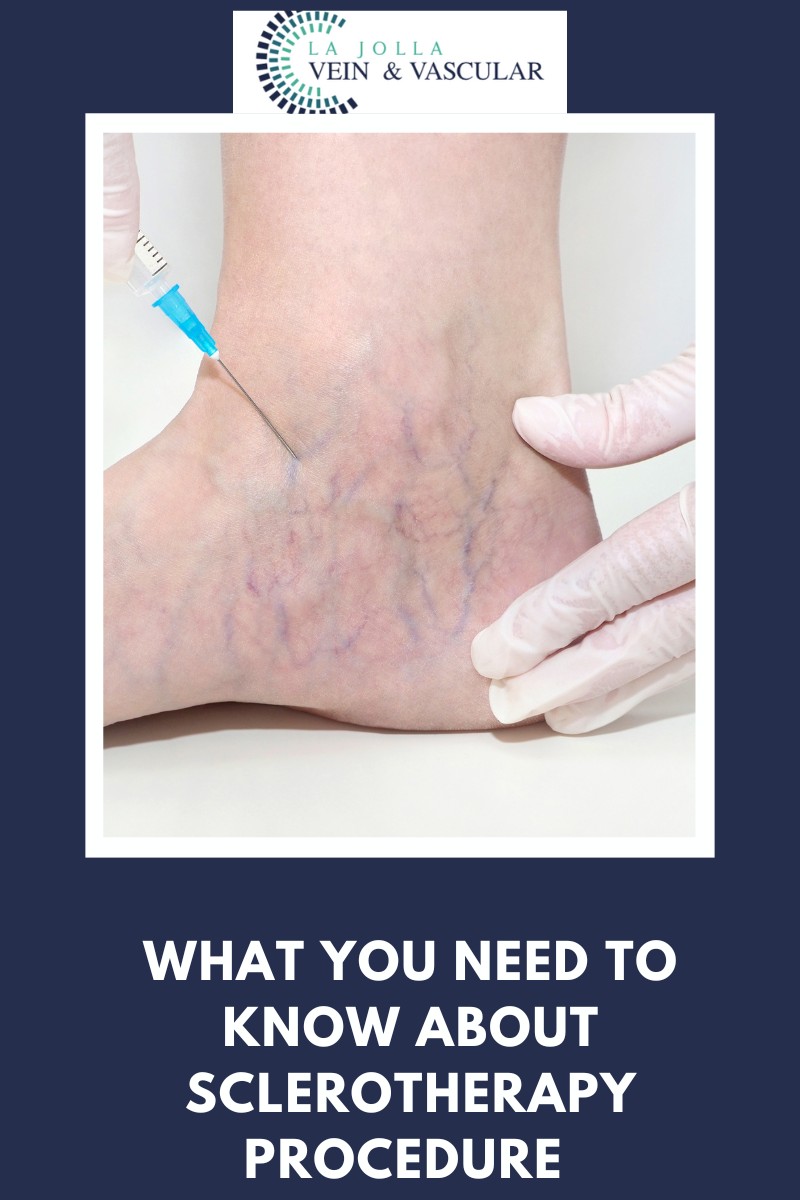
LJVascular2022-07-16T18:32:09-07:00Today, sclerotherapy is clearly the gold standard for removing spider and varicose veins. During this procedure, a specially trained physician injects a safe sclerosing agent directly into the blood vessel. The effectiveness of the procedure comes as a direct result of the training, experience, and judgment of the physician to make sure that the sclerosant’s volume, concentration, and exposure time are exactly right.
What happens next? The solution displaces the blood in the vein, causing it to immediately appear lighter in color. The solution irritates the vein lining, causing it to collapse and blocking it from receiving more blood. Within a few weeks, the unused vein is absorbed by the body and disappears. With advancements in medicine, there’s no reason to go under the knife anymore—sclerotherapy is a safe, effective, and cost effective alternative to surgery.
Sclerotherapy Treatment for Spider Veins
Spider veins and reticular veins of the legs are most commonly treated with sclerotherapy. Sclerotherapy involves an injection of a medication into the vein. This will cause the vein to collapse and gradually fade away. Sclerotherapy has been used to treat spider veins for decades, but newer solutions such as AscleraTM allow for spider veins to be treated with minimal discomfort and immediate return to activities. Vein specialists rarely use saline solutions these days, because alternative solutions are less painful and better tolerated. Sclerotherapy is preferred by most vein specialists over laser because spider veins often have underlying ‘feeder veins’ that can easily be treated with sclerotherapy, but are not addressed by laser. Many people will require more than one treatment session for optimal results. The national average is 2 to 5 treatment sessions. Treatment sessions are often spaced a month apart, but your health care provider will help determine your customized care plan. Wearing compression stockings after treatment will improve results.
For larger veins, the medication may be turned into a foam, this is referred to as foam sclerotherapy. Foam sclerotherapy is similar to sclerotherapy of spider veins but instead of a liquid solution, a foamed-solution is injected directly into the vein via a small needle. The solution can be seen on ultrasound monitoring which allows it to be directed into nearby varicose veins painlessly. The veins will seal shut, and gradually be broken down by the body.
Below are a few patient cases after Sclerotherapy Treatment which you will see the before and after results.
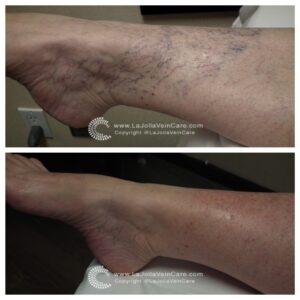
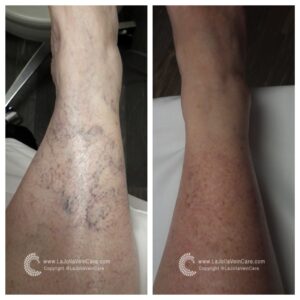
If you experience any vein disease symptoms, please call our office at (858)-434-5998 to schedule a consultation with one of our knowledgeable doctors at La Jolla Vein and Vascular.
For more information on vein health please check out our Youtube Channel or visit our helpful guide of resources.