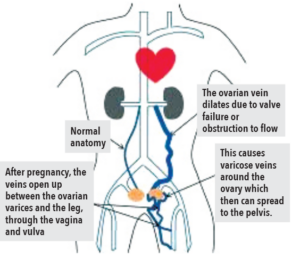
Testing and Diagnosis of Pelvic Varicose Veins
How are Pelvic Varicose Veins Diagnosed?
From the list shared previously regarding the common symptoms and signs associated with pelvic congestion syndrome, you can tell most are either common or can be easily misdiagnosed. For example, if you are having recurring back pain, you could easily get some pain relievers thinking that to be the problem.
Medically, doctors may need to run a number of tests before diagnosing the condition. This is a result of the various associative symptoms. Moreover, since there’s such a vast array of symptoms, healthcare providers need to rule out other possible underlying causes for the symptoms.
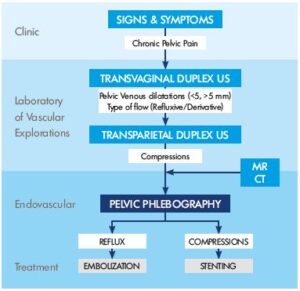
Some of the procedures you can expect when getting vulvar varicose veins include;
A laparoscopy: This is a relatively small and minimally invasive surgical procedure where the doctor inserts a small camera inside the pelvis for a clearer and objective look.
A computed tomography (CT) scan
A Magnetic Resonance Imaging Scan (MRI)
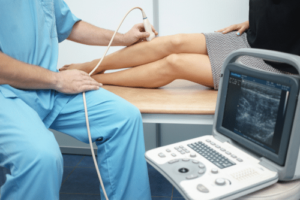
An ultrasound tests
A venogram exam
In most cases, the healthcare provider will opt for the ultrasound examination. Besides being simple, non-intrusive, and quick, an ultrasound exam can detect varicosities and assess the blood flow.
Seeing a doctor can prove beneficial, even when you are exhibiting some or none of the apparent symptoms. This is largely because some women with developing labial varicosities show little to no symptoms other than swollen veins.
The other importance of seeing a doctor whenever you start exhibiting these signs is to get ahead of any underlying health conditions. Pelvic congestion syndrome is often the sign of other health issues, especially regarding the body’s circulatory system. For instance, through an examination, pelvic varicose veins could help identify varicose veins in other parts of the body.
Are Vulvar Varicosities Permanent?
Pelvic congestion syndrome is rarely a permanent condition. Most of the symptoms will likely disappear within six to eight weeks of giving birth.
However, if you have previously developed labial varicosities during a previous pregnancy, chances are high the condition will come back during the next pregnancy. In these cases, the recurring pelvic congestion syndrome will be more painful with every subsequent pregnancy.
Even when the varicosities disappear on their own, it’s still vital to speak with your doctor. This will help kick in preventative measures to ensure the condition doesn’t recur.
Are Labial Varicose Veins Treatable?
So, you’ve noticed a few worrying signs, gone to the doctor, had tests run, and the results are out; you have pelvic congestion syndrome. What next?
Well, the treatment approach largely depends on whether you are pregnant or not. If you are pregnant, the best cause of action is alleviating the pain and discomfort and eliminating the symptoms. The treatment option for pregnant women is aimed at alleviating any pain and accompanying symptoms. To achieve this, the healthcare provider may use various medications, including;
Nonsteroidal anti-inflammatory drugs (NSAIDs)
Chronic pain relief medication such as gapapentin and amitriptyline
In other cases, the faulty veins can be targeted, isolated, then closed off through minimally invasive procedures. Once these nonfunctional veins are closed, the body will naturally redirect venous blood to the healthier veins. Subsequently, the pelvic venous drainage will improve over time, taking away most, if not all, of the symptoms.
However, before these procedures are performed, your doctor may put you in an observation period lasting between six to twelve months. Since most varicosities disappear after eight weeks, the doctors may choose to give your body a chance to repair itself. FOrtunately, you can still receive pain medication to alleviate any pain during this observation window. You can also use various anecdotal remedies include;
Avoid standing or sitting for too long
Avoid wearing uncomfortable shoes, such as high heels, which put more pressure on your lower body and back
Change positions regularly
Drink a lot of water
Elevate your legs periodically to improve blood circulation
Applying heat or ice on the painful areas
Wearing supportive underwear when pregnant-such as compression and support stockings while labial varicose veins are not usually dangerous, may lead to poor circulation in the lower parts of your body. This could then lead to blood pooling, which can cause deep vein thrombosis.
When these blood clots are in the deeper veins, they can break loose and move to other parts of the body. These cases, while rare, can lead to life-threatening complications.
Some of the signs of blood clot development include increased pain in the affected region, redness, swelling, and hardening. If you experience any of these, you should notify your healthcare provider as soon as possible.
Labial Varicose Veins
Unlike varicose veins, spider veins are harmless. Most people seek treatment for cosmetic reasons. However, treatment will also alleviate the mild yet persistent discomfort this condition sometimes causes.
So, if this is you and you’ve been experiencing pain, please give our office a call at 858-550-0330.
For more information please check out our Youtube Channel at this link.