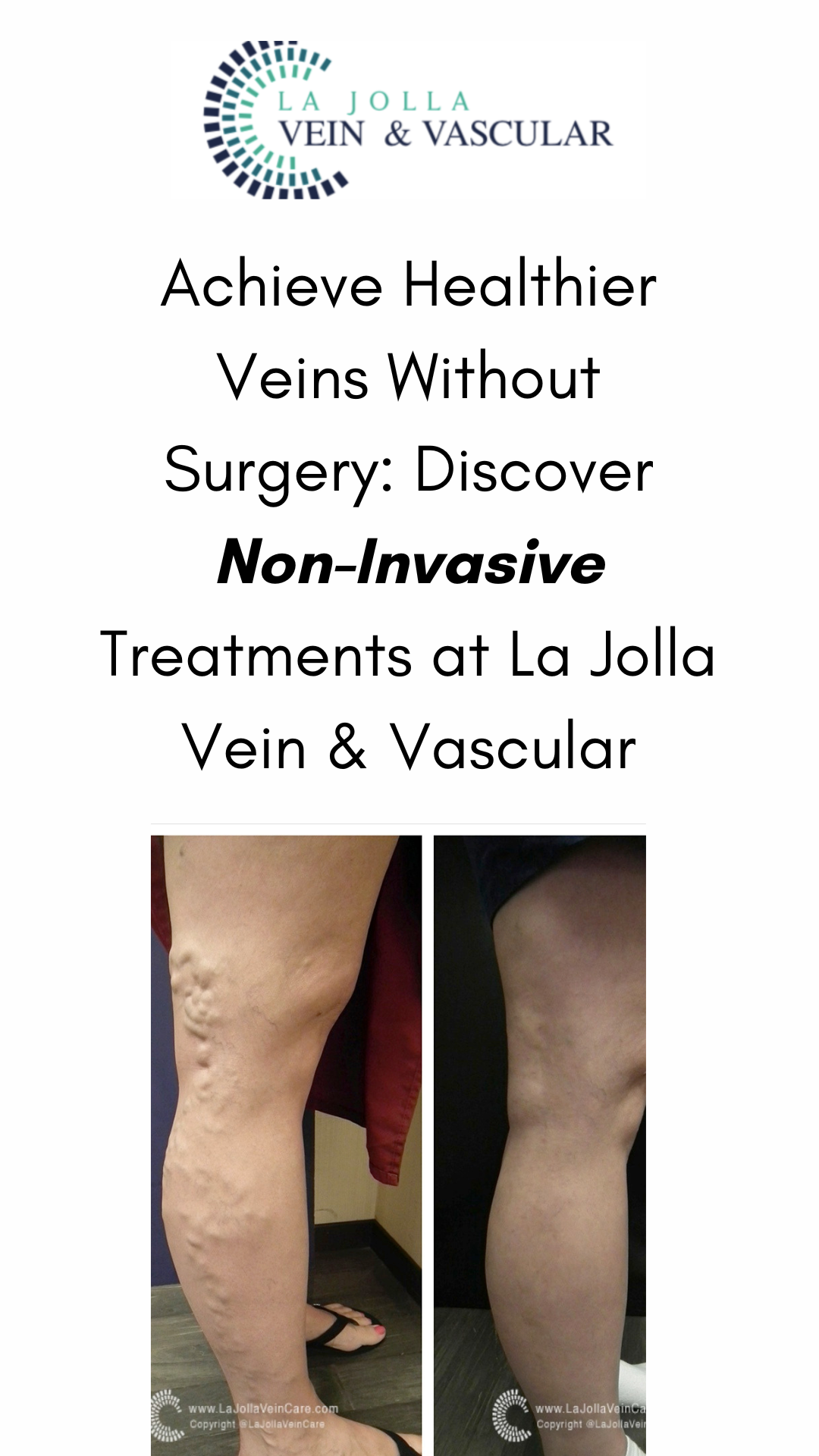
From Discomfort to Confidence: Patient Transformation Stories in Varicose Vein Treatment
LJVascular2024-10-23T18:24:00-07:00From Discomfort to Confidence: Patient Transformation Stories in Varicose Vein Treatment
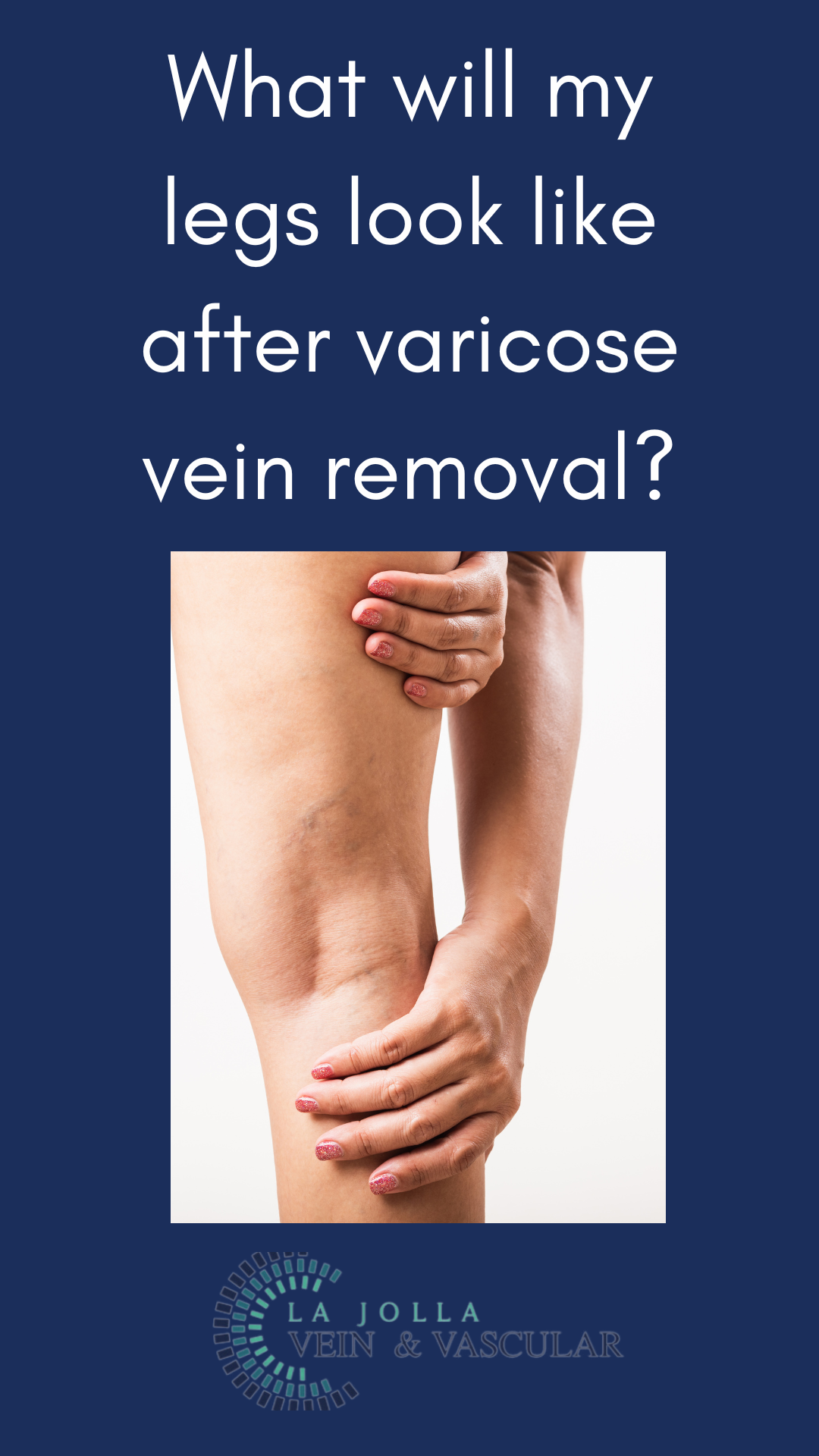
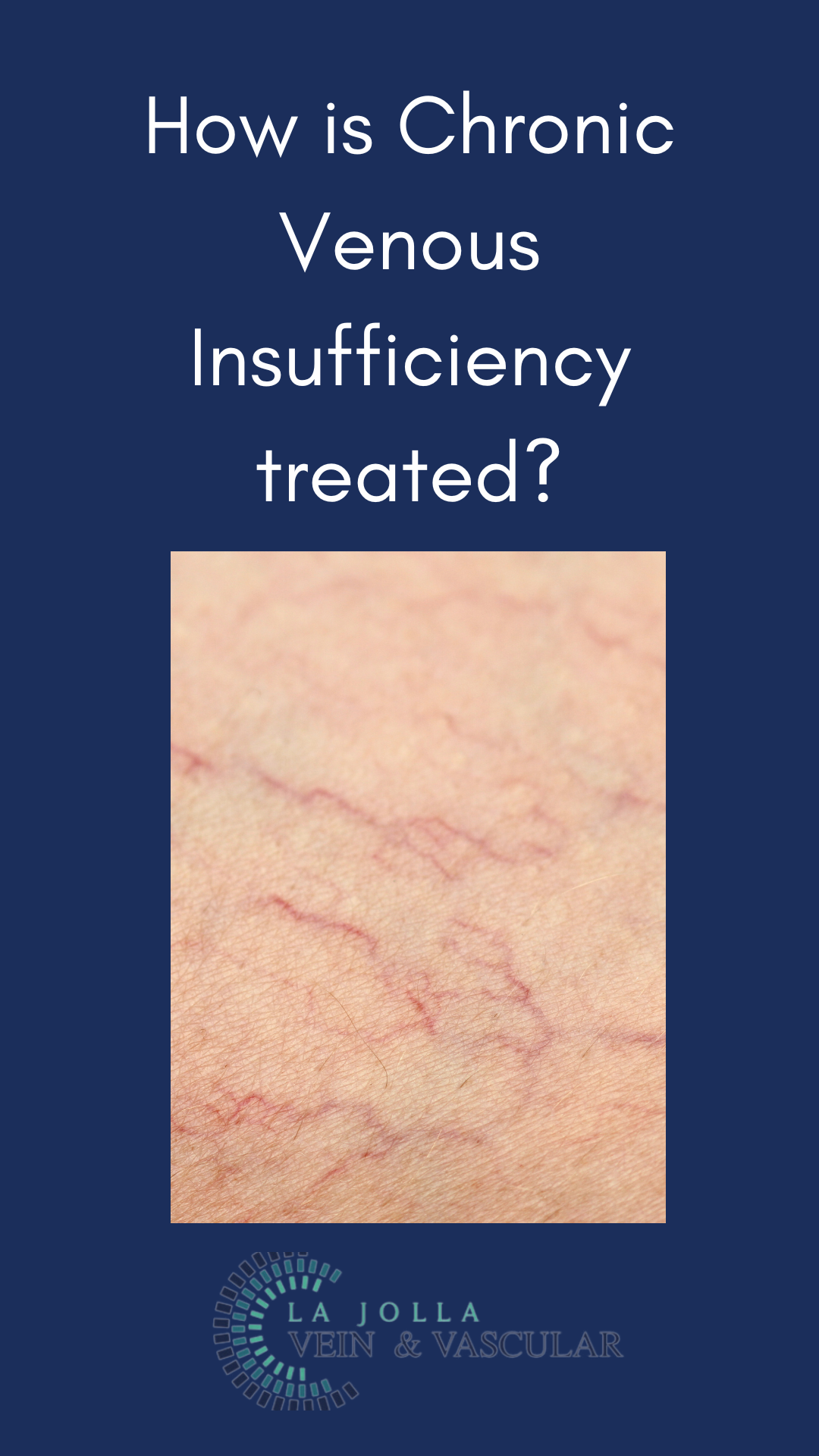
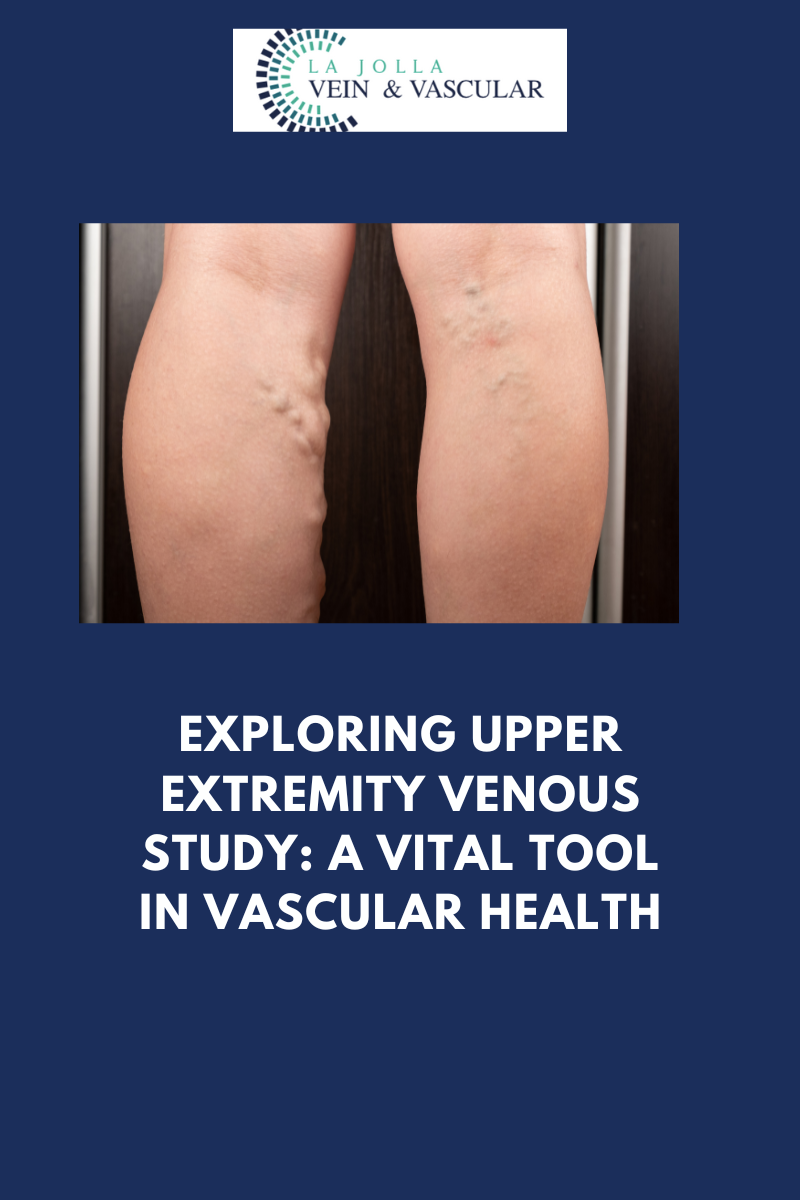
Varicose veins, those unsightly, swollen veins lurking just beneath the skin’s surface, can be a cause for concern among many individuals. While they most commonly make their appearance on the legs, these pesky veins can manifest elsewhere in the body. In […]