Transform Your Vein Health with Minimally Invasive Treatments at La Jolla Vein & Vascular
LJVascular2024-06-06T10:30:21-07:00At La Jolla Vein & Vascular, we pride ourselves on leading the way in non-surgical minimally invasive vein treatments, offering exceptional results without invasive procedures. Our commitment to excellence and patient satisfaction shines through in the numerous success stories of those who have experienced remarkable improvements in their vein health and overall well-being with our non-surgical methods.
Expertise in Minimally Invasive Vein Treatments
Our highly qualified team specializes in non-invasive techniques, providing a comfortable and stress-free environment for treatments that require no incisions or cutting. By utilizing advanced methods to collapse problematic veins, we enable them to dissolve naturally over time. This modern approach eliminates the need for surgical incisions, significantly reducing discomfort and downtime.
Convenient and Efficient In-Office Procedures
One of the major benefits of our non-surgical treatments is that they can be performed in-office without the need for general anesthesia. Patients can undergo vein treatments confidently, knowing they can return to their normal activities almost immediately. Whether you have a demanding work schedule or an active lifestyle, our treatments ensure minimal disruption to your daily routine with our minimally invasive treatments.
Transformative Results
The outcomes of our non-surgical treatments are truly transformative. As the treated veins collapse, damaged veins disappear from the skin’s surface, and blood flow is redirected through healthier veins. This not only enhances the appearance of your legs but also alleviates symptoms such as pain, swelling, and discomfort. Our patients often experience a renewed sense of confidence and vitality, allowing them to fully embrace an active and healthy lifestyle.
Testimonials and Success Stories
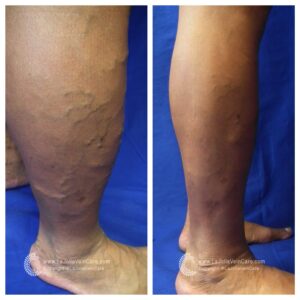
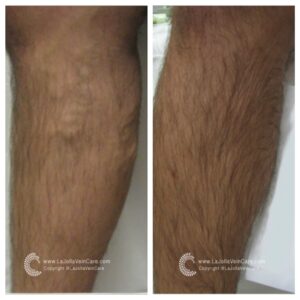
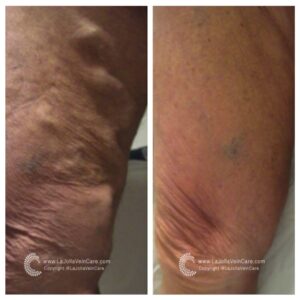
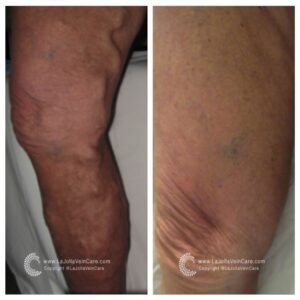
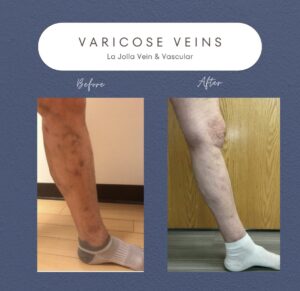
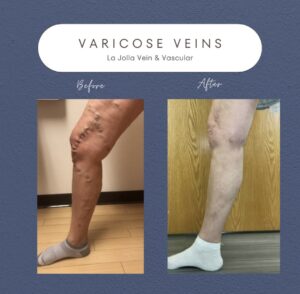
Don’t just take our word for it—our patients’ testimonials and before-and-after photos highlight the effectiveness of our non-surgical treatments. From individuals who have struggled with varicose veins for years to those seeking preventive care, our patients consistently report positive outcomes and life-changing experiences. Their stories are a testament to the power of non-surgical treatments in restoring vein health and enhancing overall quality of life.
See the Transformations for Yourself
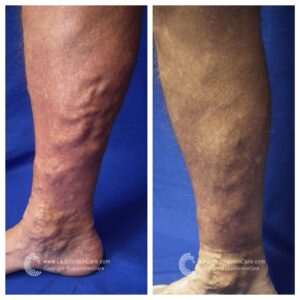
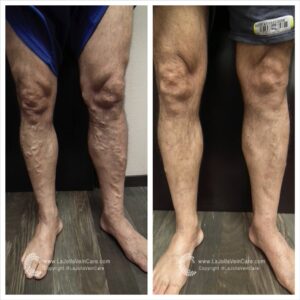
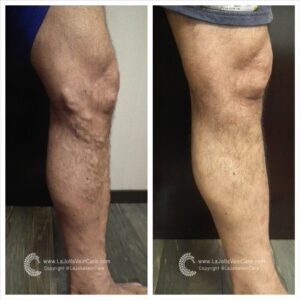
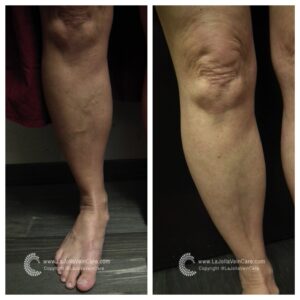
By showcasing our patients’ before-and-after transformations, we aim to inspire hope and confidence in others dealing with vein issues. Whether it’s the elimination of unsightly veins or the relief of painful symptoms, our patients’ success stories demonstrate that effective solutions exist without surgery or lengthy recovery times. With the expertise of our team at La Jolla Vein & Vascular, you can take control of your vein health and enjoy the benefits of non-surgical treatments.
Committed to Exceptional Care
Our dedication to providing exceptional care and achieving outstanding results distinguishes us as leaders in non-surgical vein treatments. With our innovative approach, patients can experience remarkable improvements in their vein health and overall well-being without invasive procedures. From enhancing appearance to relieving symptoms, the benefits of our treatments are truly life-changing.
If you’re ready to experience the difference for yourself, schedule a consultation with us today and take the first step toward healthier, happier veins.
“Bringing Experts Together for Unparalleled Vein and Vascular Care”
La Jolla Vein & Vascular (formerly La Jolla Vein Care) is committed to bringing experts together for unparalleled vein and vascular care.
Nisha Bunke, MD, Sarah Lucas, MD, and Amanda Steinberger, MD are specialists who combine their experience and expertise to offer world-class vascular care.
Our accredited center is also a nationally known teaching site and center of excellence.
For more information on treatments and to book a consultation, please give our office a call at 858-550-0330.
For a deeper dive into vein and vascular care, please check out our Youtube Channel at this link, and our website https://ljvascular.com
For more information on varicose veins and eliminating underlying venous insufficiency,
Please follow our social media Instagram Profile for more fun videos and educational information.
For more blogs and educational content, please check out our clinic’s blog posts!