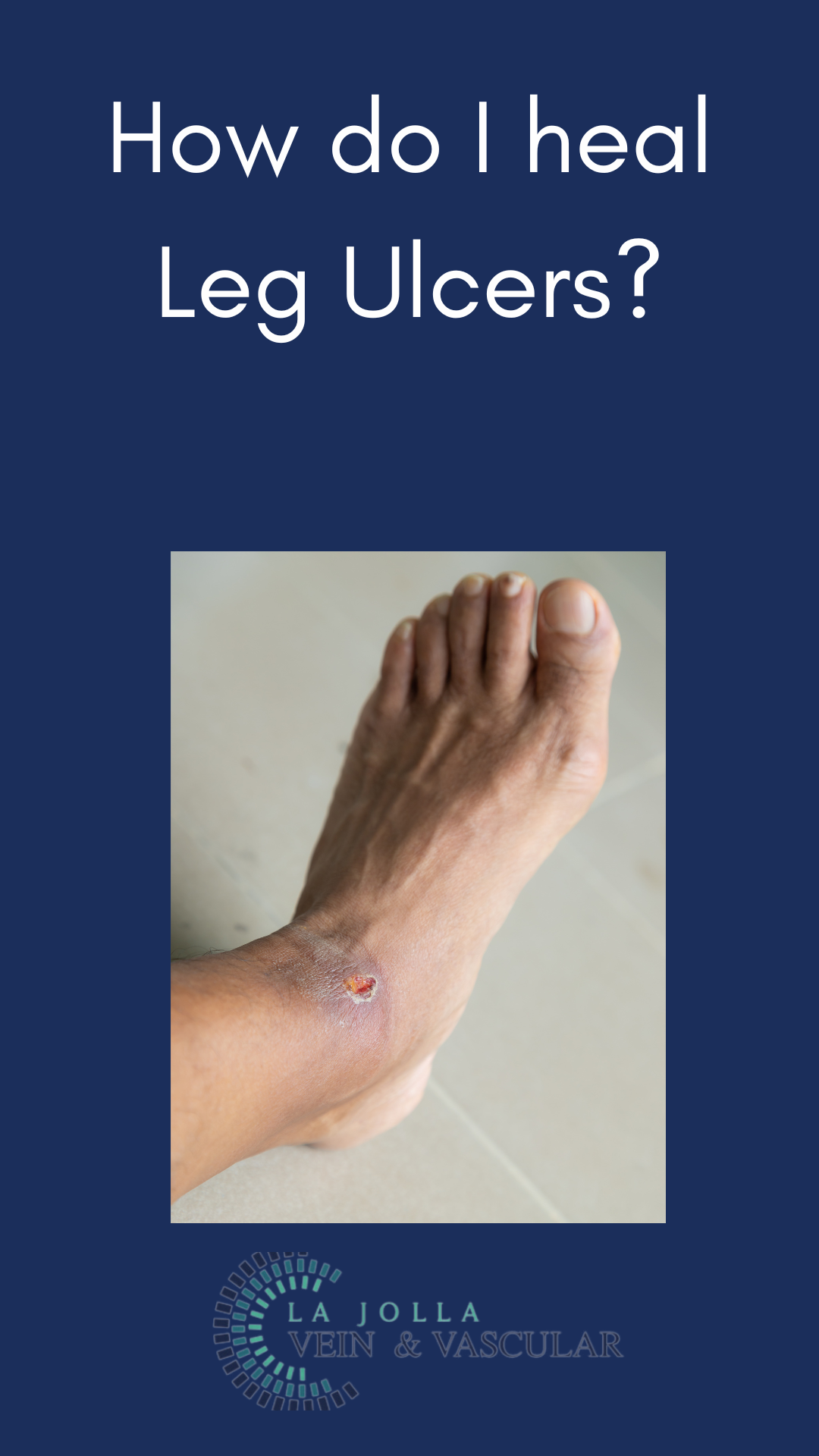
From Wounds to Wellness: Healing Leg Ulcers with Venous Disease Management
LJVascular2024-10-23T05:47:52-07:00From Wounds to Wellness: Healing Leg Ulcers with Venous Disease Management
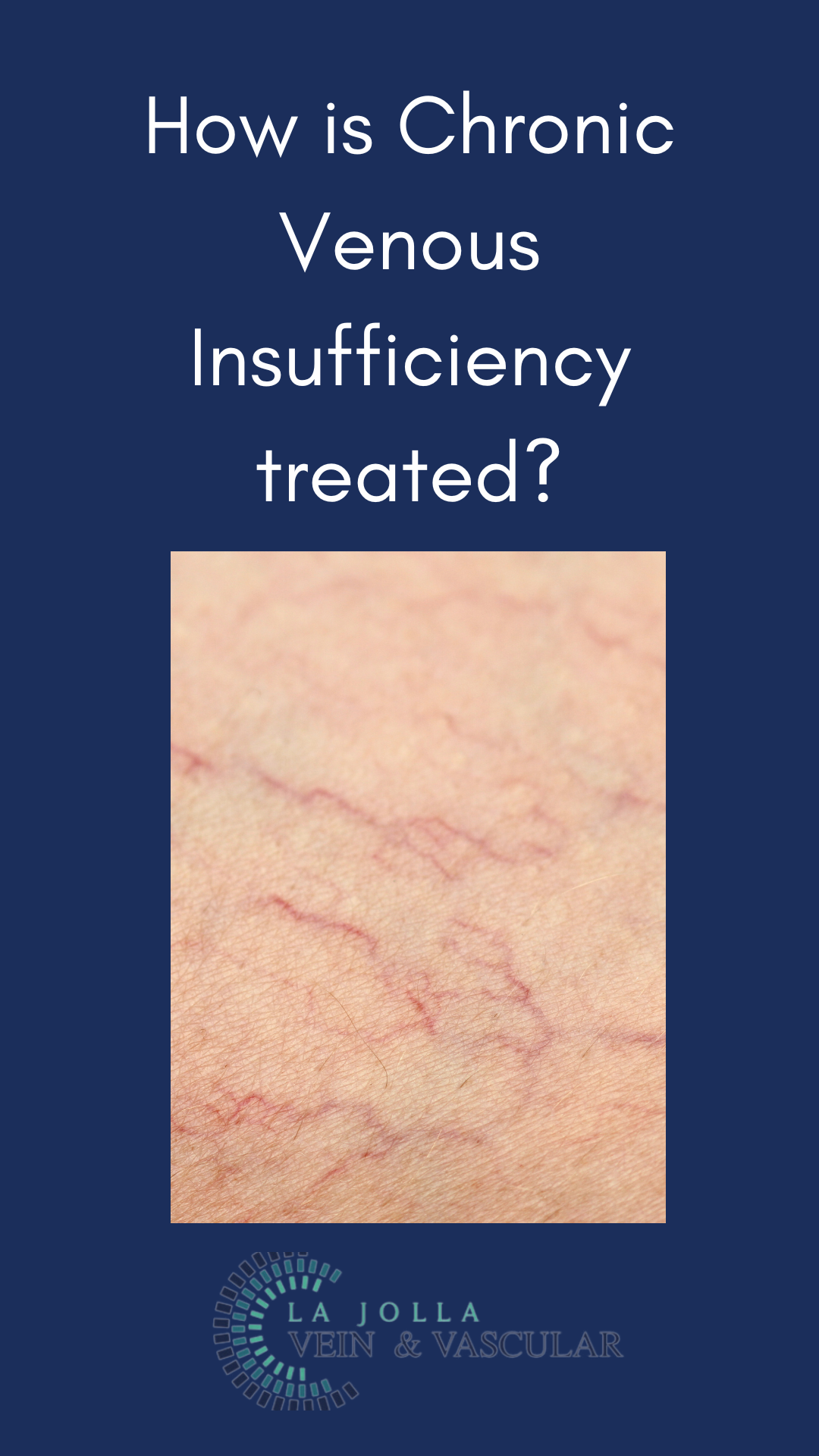
In the realm of vascular health, chronic venous insufficiency (CVI) stands as a prevalent yet often misunderstood condition including leg ulcers. Characterized by a cascade of […]