RFA for perforator vein reflux
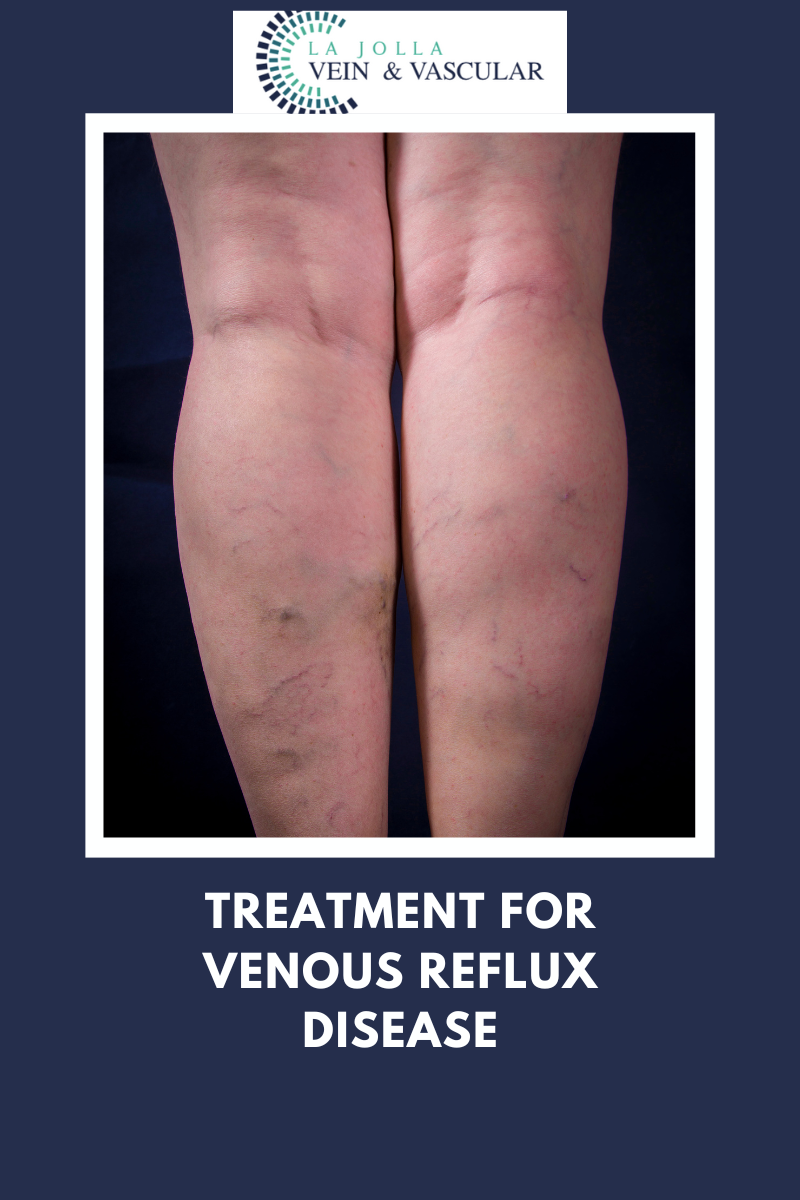
LJVascular2023-05-24T16:56:04-07:00Radiofrequency perforator ablation (RFA) is performed on perforator veins, short connections between your deep and superficial veins. Perforator veins can suffer the same sort of valve damage and retrograde blood flow (venous reflux) as other veins. Most patients with vein disease who experience skin changes, (that also may result […]