Self Care 101 for Varicose Veins
LJVascular2024-06-09T01:42:36-07:00Conservative Management and Self-Care for Varicose Veins
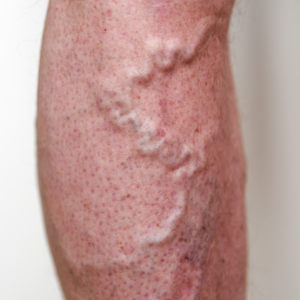
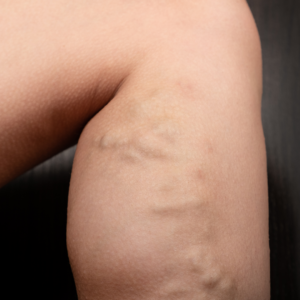
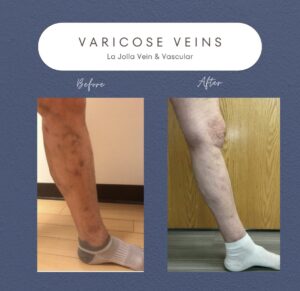
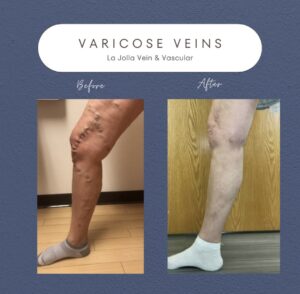
Varicose veins can cause discomfort and lead to complications such as thrombophlebitis (blood clots within veins) and vein rupture. While conservative management and lifestyle changes can’t make varicose veins disappear, they can ease symptoms and help reduce the risk of complications. These measures are especially helpful for […]