Chemical solutions for vascular wellness: Exploring the Ablation procedure
LJVascular2024-10-31T22:28:04-07:00Chemical Solutions for Vascular Wellness: Exploring the Ablation Procedure
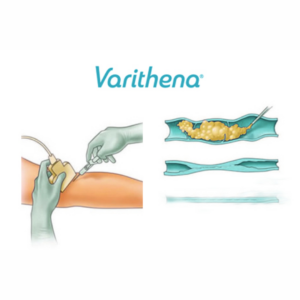
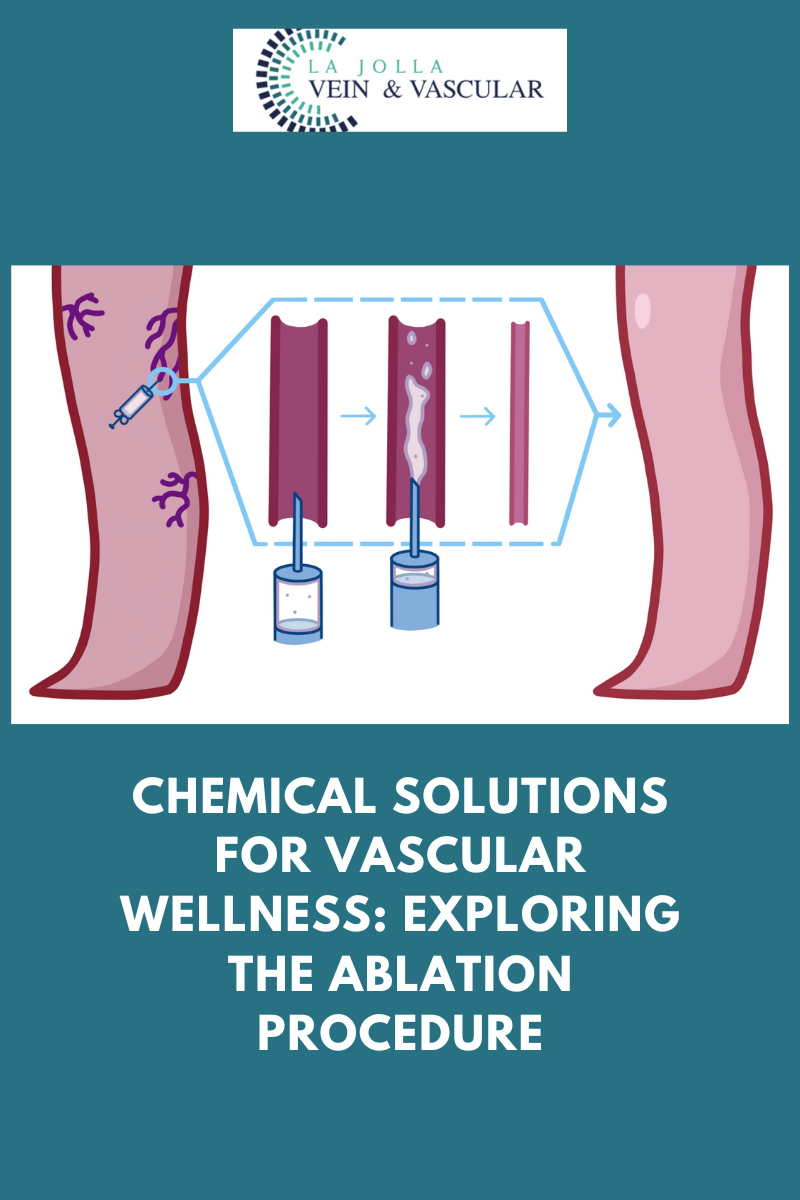
Unveiling Varithena: Advancing Vein Health with Injectable Foam Treatment
In the realm of modern vein treatments, Varithena (ablation procedure) emerges as a groundbreaking solution for addressing varicose veins within […]