Effective Solutions for Spider Veins: Non-Surgical Treatment at La Jolla Vein & Vascular
LJVascular2024-06-06T07:29:32-07:00Effective Solutions for Spider Veins: Non-Surgical Treatment at La Jolla Vein & Vascular
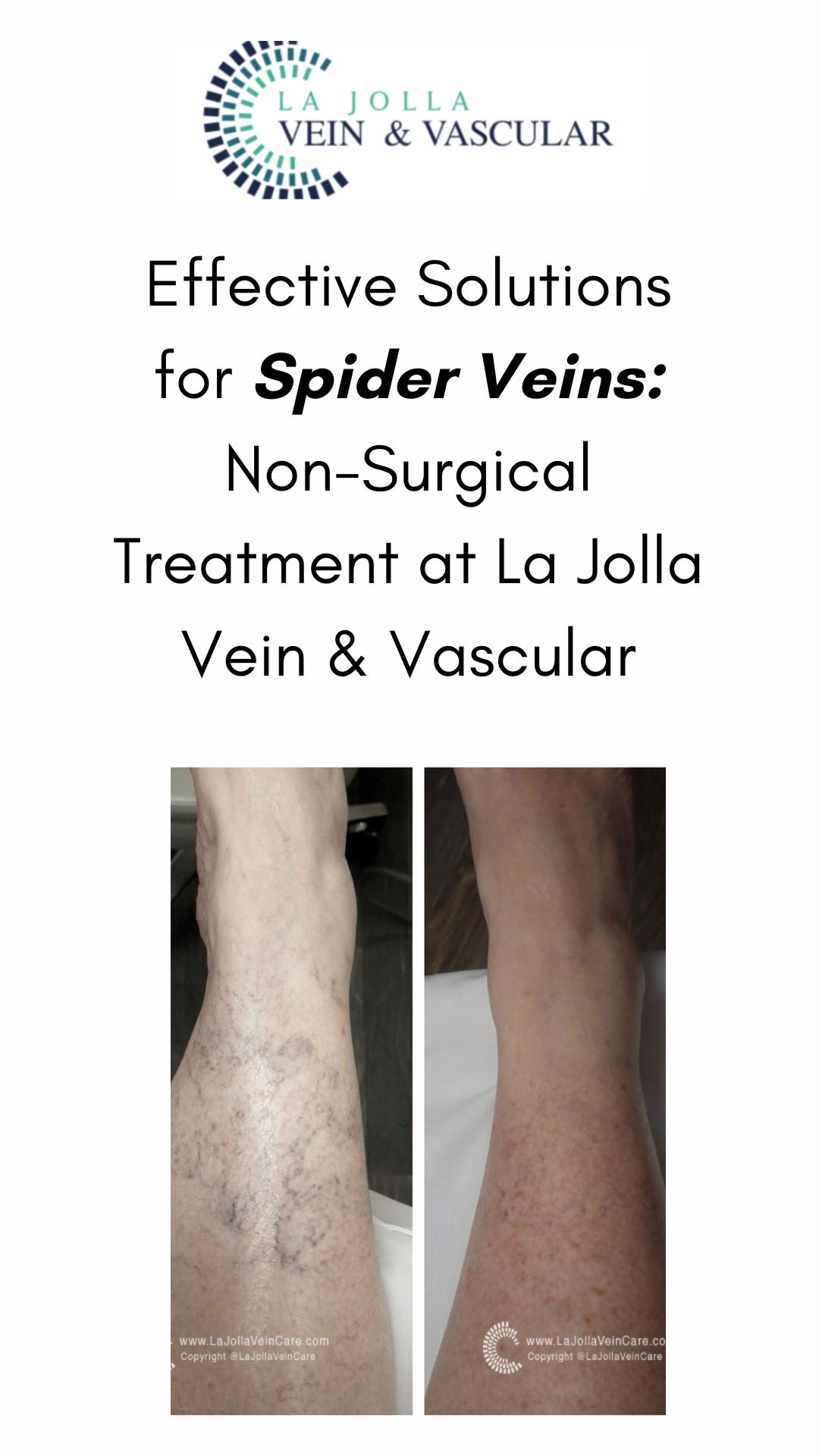
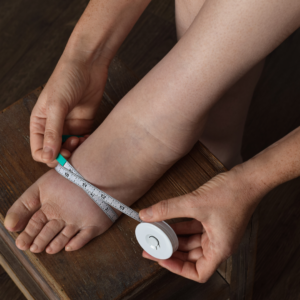
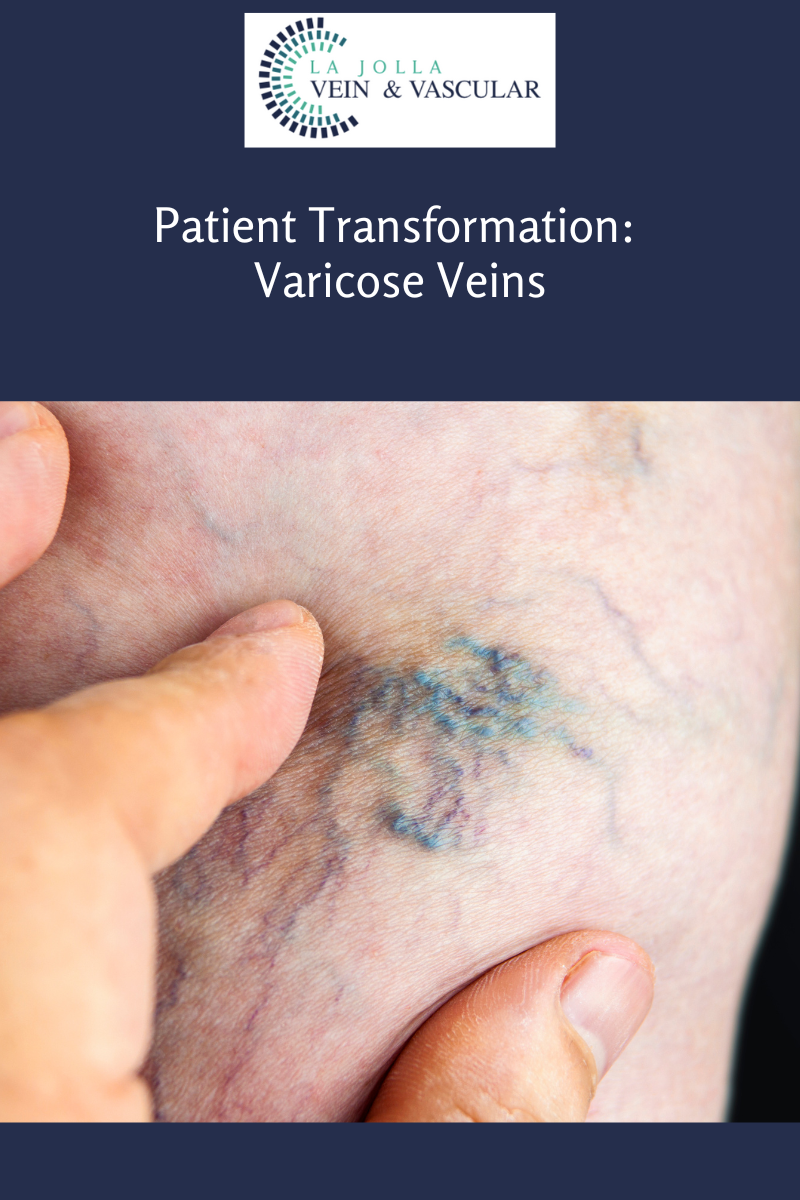
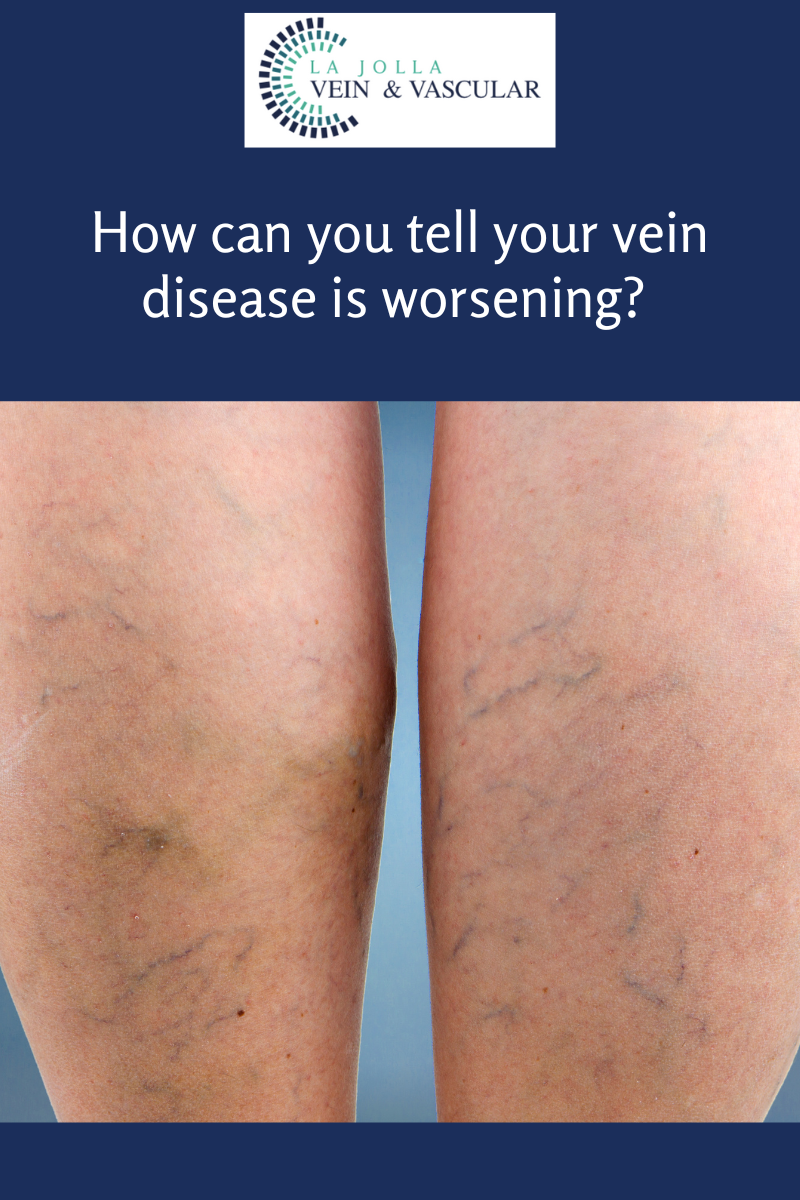
What are spider veins?
Spider veins are the fine, thread-like reddish veins at the surface of the skin. These veins are not healthy. Veins are often considered a cosmetic issue, but they can be associated with underlying feeder veins, not […]