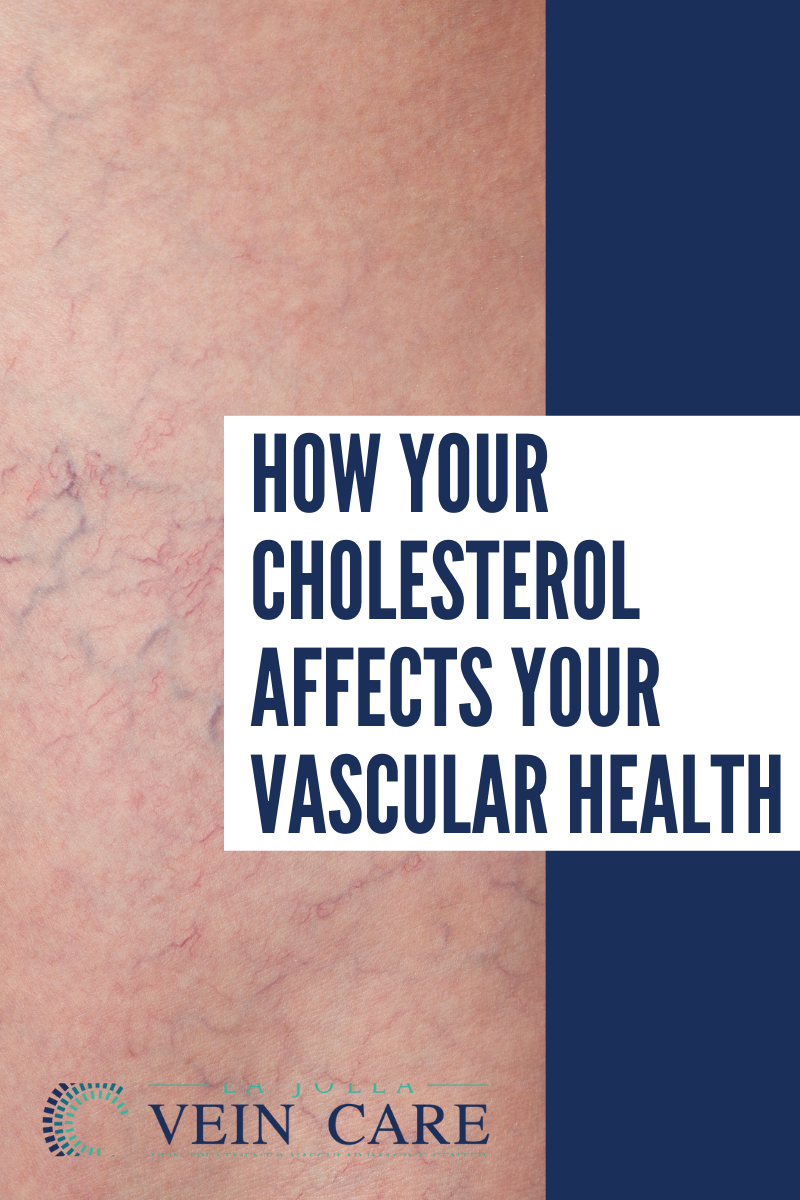
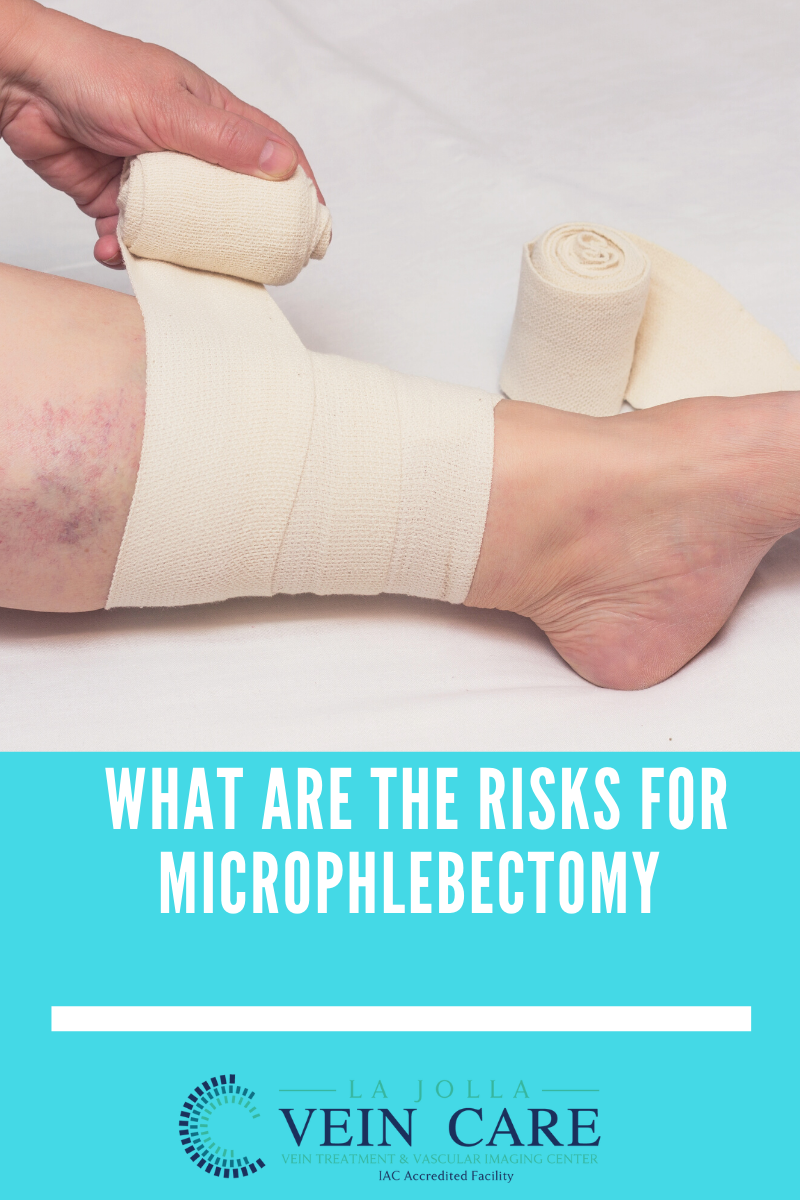
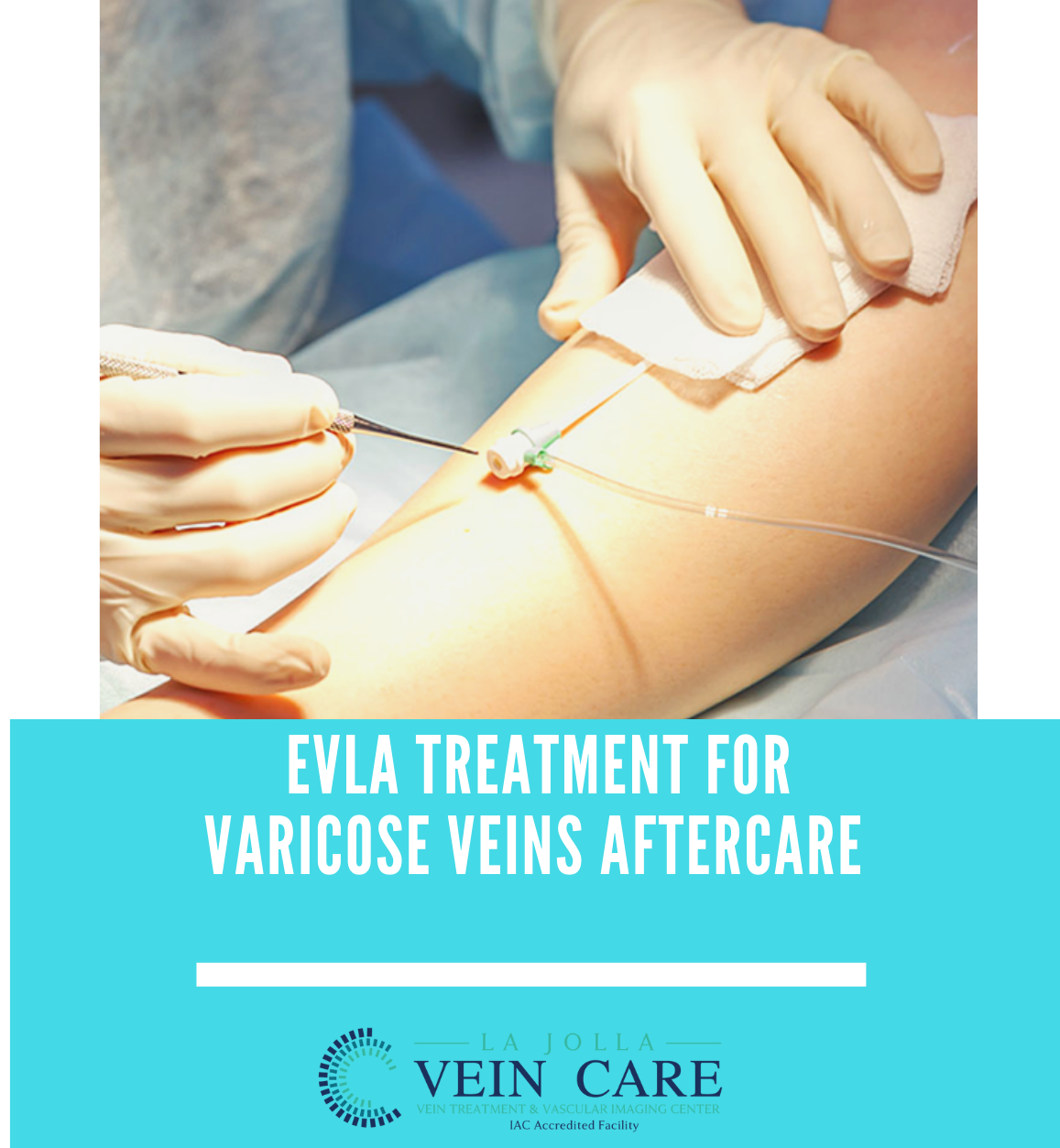
What are Non Healing Ulcers & Wounds?
LJVascular2022-04-28T17:17:13-07:00Non-Healing Ulcers & Wounds
We might all be familiar with non healing ulcers & wounds in a general manner, but certain types of ulcers behave quite differently due to various contributing factors. These are non healing ulcers or non healing wounds, and if not treated with care and in good time, such wounds can […]