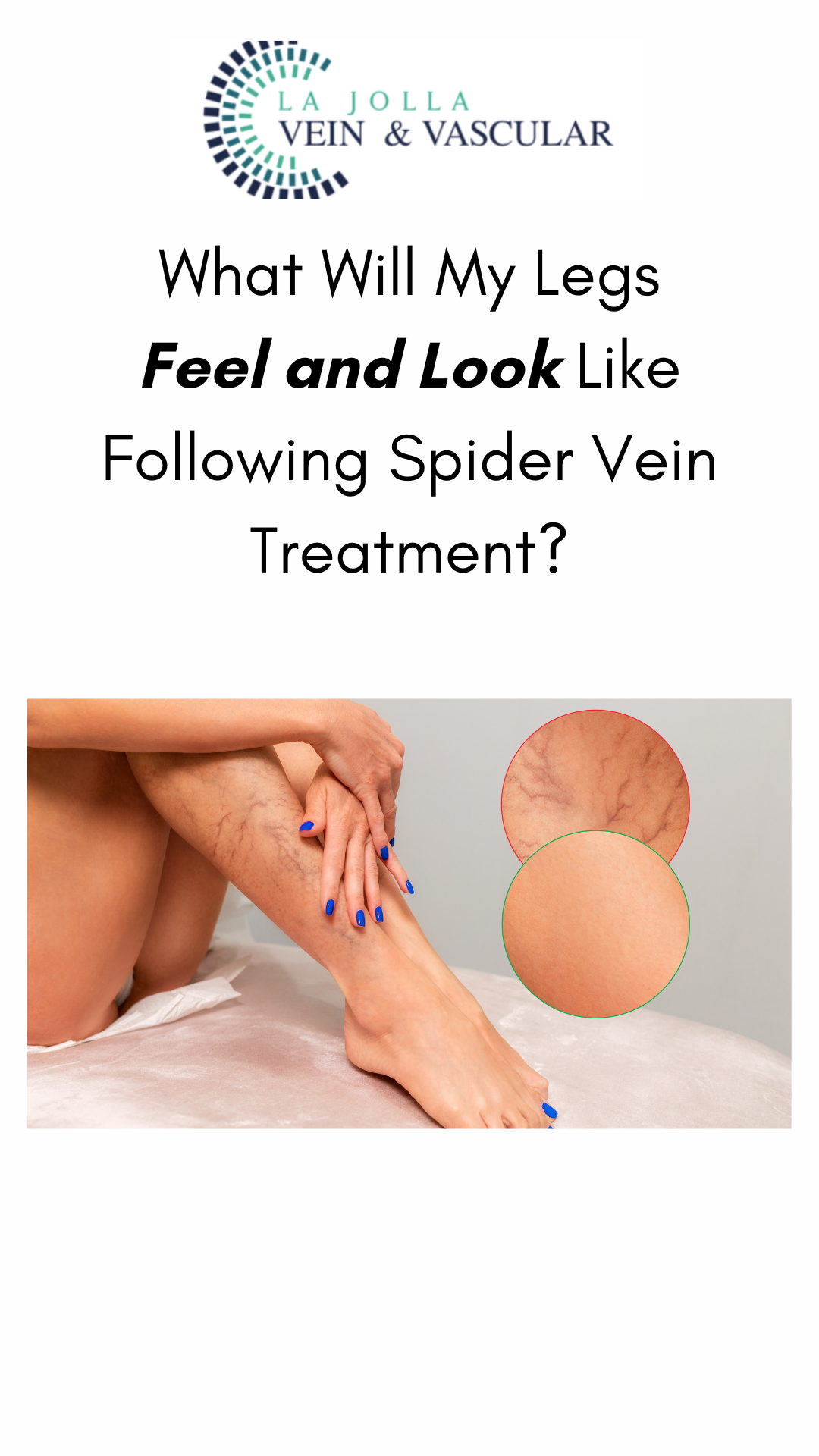
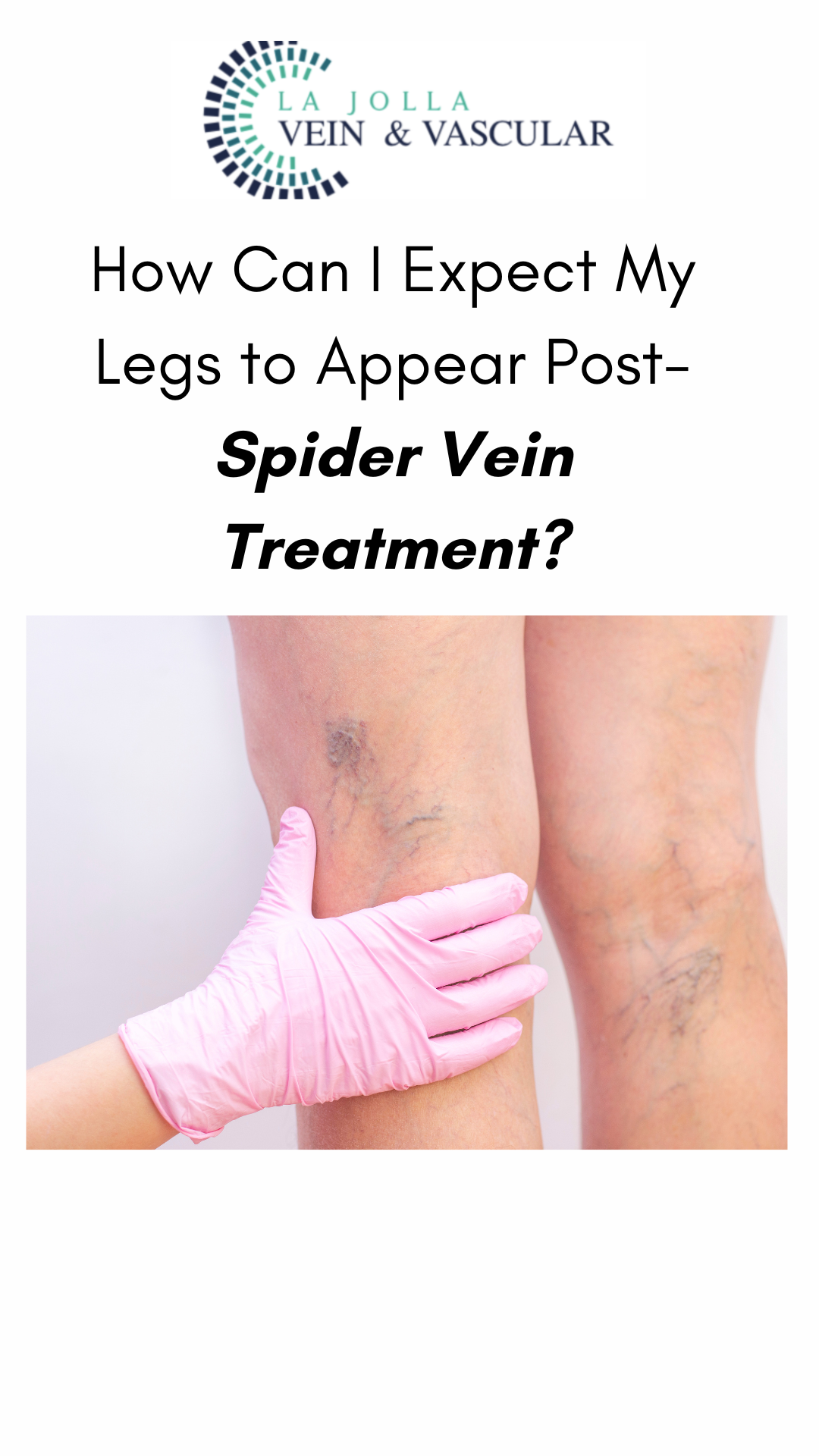
What Will My Legs Feel and Look Like Following Spider Vein Treatment?
LJVascular2024-06-03T06:53:02-07:00At La Jolla Vein Care, we take pride in our pioneering non-surgical vein treatments that deliver outstanding results, transforming the vein health and overall well-being of our patients without the need for invasive procedures. With a highly qualified staff proficient in non-invasive techniques, we offer a comfortable environment where patients can undergo […]