Venous Duplex Ultrasound: Peering Beneath the Surface for Vascular Clarity
LJVascular2024-07-07T02:22:48-07:00Venous Duplex Ultrasound: Peering Beneath the Surface for Vascular Clarity
In the realm of understanding and diagnosing vein and vascular diseases, cutting-edge medical technology plays a pivotal role in uncovering the mysteries hidden beneath the surface. Among the most invaluable tools in this domain is Duplex Ultrasound. In this blog post, we embark on a journey to demystify Duplex Ultrasound, shedding light on its applications, advantages, and the pivotal role it plays in diagnosing and managing vein and vascular diseases.
Decoding the Enigma of Duplex Ultrasound
Duplex ultrasound is a specialized imaging technique that ingeniously combines two indispensable components: the traditional ultrasound (referred to as B-mode) and Doppler ultrasound. This amalgamation of technologies empowers healthcare professionals to not only visualize the structure of blood vessels but also assess the flow and speed of blood coursing within them.
The Versatility of Duplex Ultrasound
Duplex Ultrasound emerges as a versatile diagnostic tool, serving a multitude of purposes. Let’s navigate through some of its primary applications and advantages:
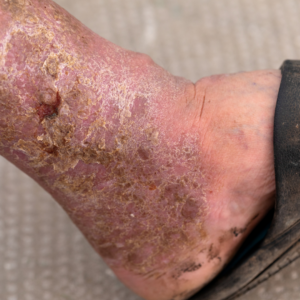
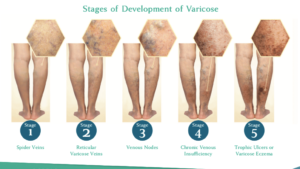
- Detecting Vein Diseases: Duplex Ultrasound assumes a pivotal role in pinpointing various vein conditions, including varicose veins, deep vein thrombosis (DVT), and chronic venous insufficiency. By providing a visual portrayal of veins and scrutinizing blood flow, healthcare practitioners can identify irregularities and formulate precise diagnoses.
- Assessing Arterial Conditions: Arterial maladies like peripheral arterial disease (PAD) and carotid artery disease yield to effective evaluation through the utilization of Duplex Ultrasound. This tool aids in recognizing arterial constriction, plaque accumulation, and blood flow obstructions, thereby contributing to timely medical interventions.
- Guiding Interventional Procedures: Duplex Ultrasound emerges as invaluable for steering minimally invasive vascular interventions such as angioplasty and stent placement. Real-time imaging empowers physicians to navigate catheters and instruments with precision, thus addressing vascular blockages effectively.
- Monitoring Blood Flow: The continual monitoring of blood flow stands as a critical necessity in numerous clinical scenarios. Duplex Ultrasound caters to this requirement, facilitating healthcare providers in evaluating the efficacy of treatments and tracking the progression of diseases.
- Non-Invasive and Painless: One of the notable merits of Duplex Ultrasound lies in its non-invasive and painless nature. Patients encounter no need for special preparations, and there are no needles or exposure to radiation involved. This renders it a secure and well-tolerated imaging modality.
- Immediate Results: Duplex Ultrasound yields real-time results, furnishing the advantage of swift assessments and instant feedback for both healthcare practitioners and patients alike. This expedites the diagnostic process and streamlines the decision-making procedure.
- Risk Assessment: The application of Duplex Ultrasound extends to evaluating the risk of potential complications, such as blood clots or aneurysms. Early detection paves the way for preventive measures to mitigate these risks effectively.
The Procedure
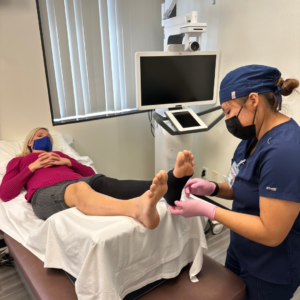
During a Duplex Ultrasound procedure, a proficient technician, often referred to as a sonographer, administers a special gel to the skin covering the targeted area for examination. This gel serves a dual purpose by facilitating the transmission of ultrasound waves while preventing any interference from air. Subsequently, a handheld device called a transducer is gently maneuvered over the skin’s surface.
The transducer emits high-frequency sound waves that bounce off the blood vessels and return as echoes. These echoes are then transformed into images and Doppler signals in color-coded fashion, presenting a holistic view of the blood vessels’ architecture and blood flow patterns.
Duplex Ultrasound emerges as a remarkable diagnostic tool that empowers healthcare providers to delve beneath the surface, unraveling crucial insights about vein and vascular diseases. Its adaptability, non-invasive attributes, and real-time imaging capabilities render it an indispensable asset in the diagnosis and management of a wide spectrum of vascular conditions.
If you or someone you know is grappling with symptoms related to vein or vascular disease, seeking guidance from a healthcare provider who harnesses the power of Duplex Ultrasound can prove to be invaluable. Such consultations can provide vital insights and steer you towards the most suitable treatment and care plan.
“Bringing Experts Together for Unparalleled Vein and Vascular Care”
La Jolla Vein & Vascular (formerly La Jolla Vein Care) is committed to bringing experts together for unparalleled vein and vascular care.
Nisha Bunke, MD, Sarah Lucas, MD, and Amanda Steinberger, MD are specialists who combine their experience and expertise to offer world-class vascular care.
Our accredited center is also a nationally known teaching site and center of excellence.
For more information on treatments and to book a consultation, please give our office a call at 858-550-0330.
For a deeper dive into vein and vascular care, please check out our Youtube Channel at this link, and our website https://ljvascular.com
For more information on varicose veins and eliminating underlying venous insufficiency,
Please follow our social media Instagram Profile and Tik Tok Profile for more fun videos and educational information.
For more blogs a