11, 4, 2021
5, 3, 2021
La Jolla Vein Care introduces Procedural Telemedicine
Web@ljvascular.com2021-11-13T16:50:59-08:00La Jolla Vein Care is pleased to announce it’s partnership with Avail Medsystems to bring the cutting edge technology of Procedural Telemedicine™ to our practice. Utilizing this collaborative equipment we can consult with remote staff and vein experts throughout the Avail network to facilitate quick, informed resolutions to even the most complicated […]
28, 6, 2020
3-Stage Approach to Vein Treatment
Nisha Bunke2020-09-17T17:58:02-07:00When visible signs of venous disease such as spider veins, varicose veins, or skin changes are present, this is usually the tip of the iceberg, and an underlying vein problem is present. An underlying vein condition (venous reflux disease) can be detected with ultrasound. A treatment plan is focused on treating the underlying vein problems […]
Park and Wait Check-In For Your Next Appointment
Nisha Bunke2020-09-17T21:35:44-07:00As part of our Vein Care Reimagined initiative, we offer Park and Wait Check In or Curbside arrival for your next appointment. This allows you to remain in your vehicle while you wait for a scheduled appointment while the staff prepares an exam room for your visit. Between each visit, exam rooms are cleaned thoroughly […]
LA JOLLA VEIN CARE EMBRACES TELEMEDICINE AND INTRODUCES REVOLUTIONARY MOBILE ULTRASOUND SERVICES AMID COVID-19 CRISIS
Nisha Bunke2025-10-15T22:44:06-07:00Telemedicine and Mobile Ultrasound Services Made Available throughout Southern California in an Aim to Ensure Important Health Concerns Don’t Go Untreated While Many Continue to Shelter in Place
LA JOLLA, CALIF. (June 9, 2020) – La Jolla Vein Care (LJVC), a leader in vein treatment serving the Southern California community for more than a decade, […]
COVID Precautions at La Jolla Vein Care
Nisha Bunke2020-09-18T02:11:40-07:00While we offer telemedicine visits and in-home ultrasound diagnostics, if you prefer or need to come to our office, we want you to know about the extensive COVID precautions we have taken to ensure our office is one of the safest places you can be.
We want you to know that our first concern has always been […]
Blood Vessel Diseases that can be Diagnosed with Duplex Ultrasound
Nisha Bunke2020-09-18T18:19:53-07:00Duplex ultrasound combines Doppler flow information and conventional imaging information, sometimes called B-mode, to allow physicians to see the structure of your blood vessels. Duplex ultrasound uses sound waves to get images of your blood vessels. It also helps determine how fast blood moves through the vessels. It can also be useful to […]
19, 5, 2020
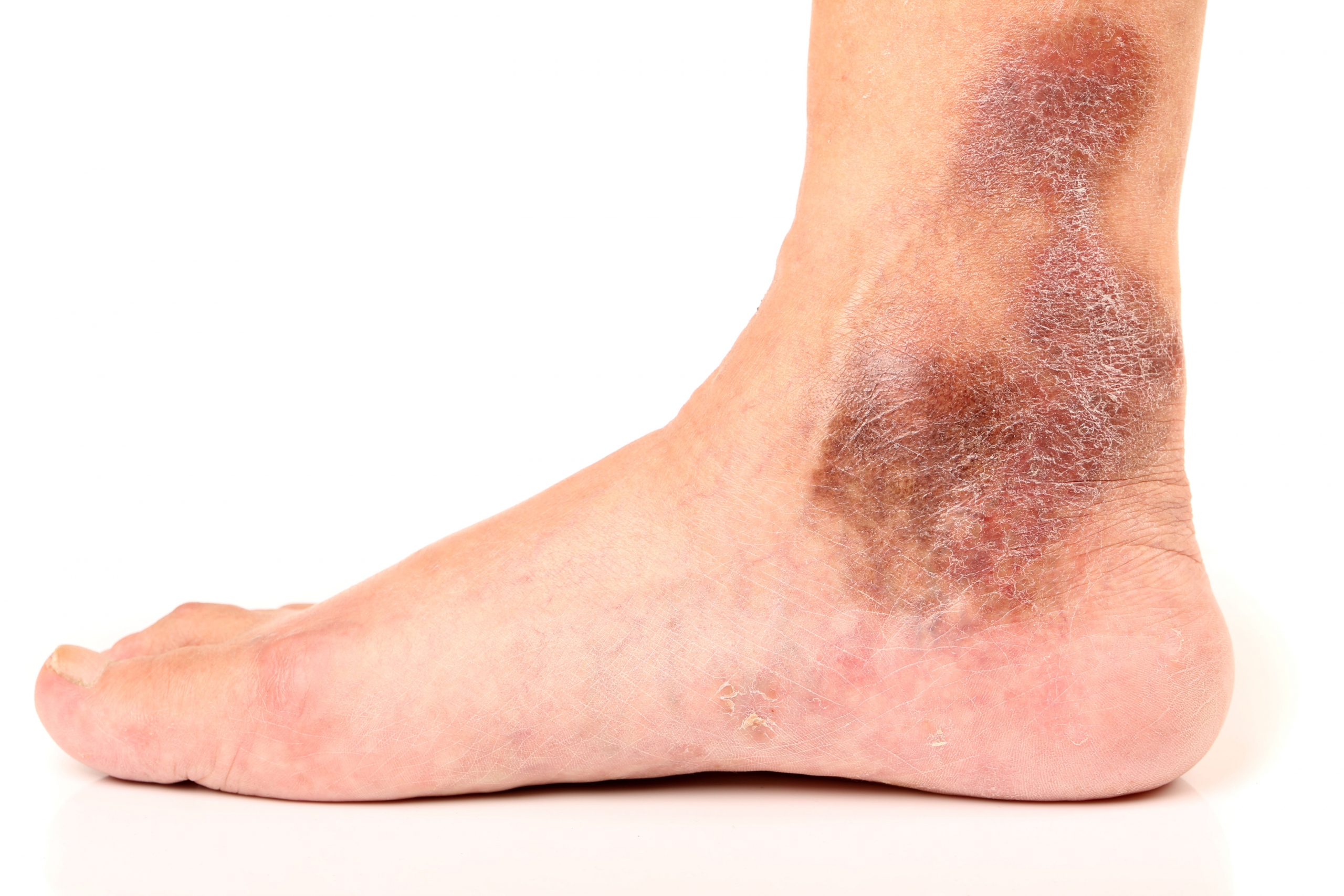
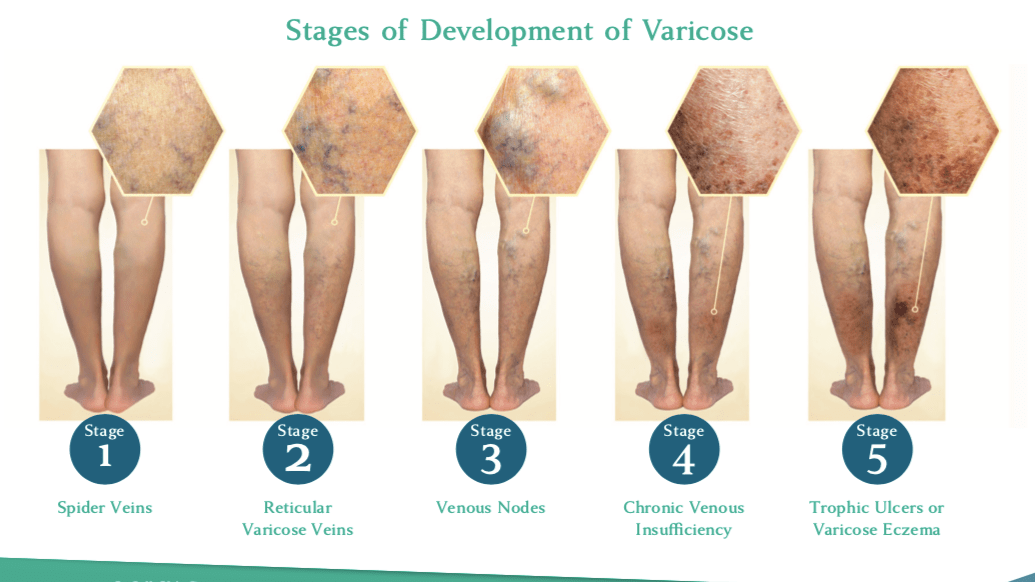
Venous Reflux is a Progressive Condition, Worsens Over Time
Nisha Bunke2025-09-04T12:26:35-07:006 Chronic Venous Insufficiency Stages
Venous reflux disease is also known as venous stasis, venous insufficiency, or venous incompetence. Venous reflux disease refers to “leaky valves” in the veins of the legs. Venous reflux may occur in the deep and/or superficial leg veins. The deep veins are those within the muscle; […]
We’re Open: Extended hours, Curb-side check-in, & Virtual Visits
Nisha Bunke2020-09-18T19:08:55-07:00We’re Open
Resuming In-office Services
La Jolla Vein Care has been actively monitoring the COVID-19 pandemic and its impact on our patient care and office protocols. Our highest priority is to continue providing the highest standard in vein care in a safe environment for our patients and staff. We have created and implemented a strategic plan using […]
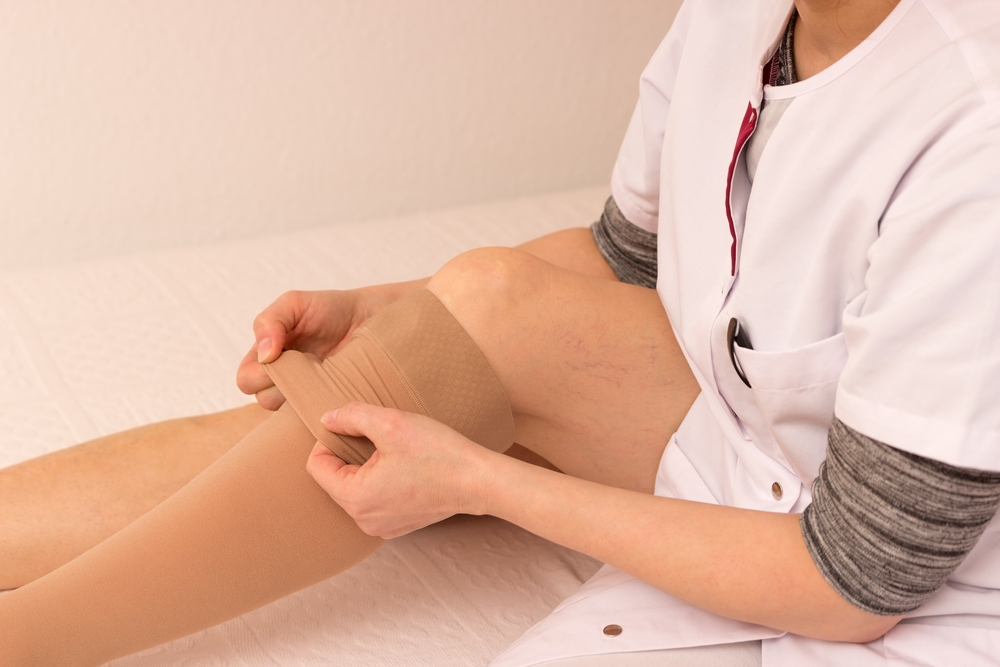
How to make compression stocking application a cinch!
Nisha Bunke2022-01-04T04:40:52-08:00- Turn your stocking completely inside out
- Locate the smaller foot hole of the stocking and tuck the foot in until you reach the heel
- Place your thumbs on either side of the tucked […]