Are there any adverse effects of vein treatment?
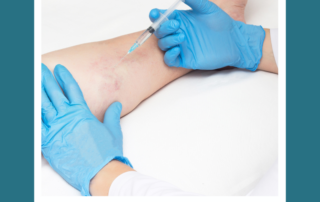
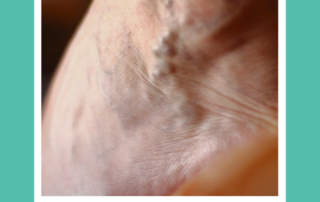
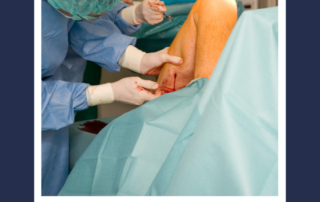
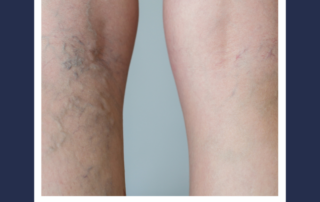
What are the adverse effects of Vein treatment?
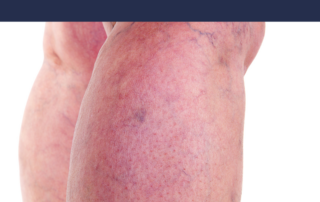
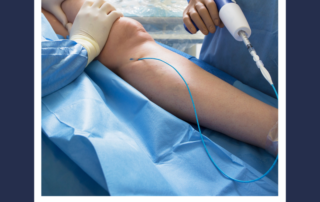
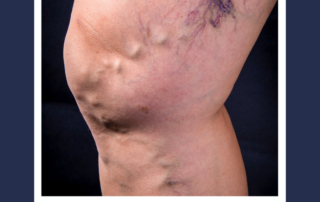
Patients generally do very well with vein treatments, all of which have a low risk of complications. Some post treatment effects can include:
Aching over the treated veins is normal after treatment. This responds well to walking, ice packs, and anti-inflammatory medications such as ibuprofen […]