La Jolla Vein & Vascular Expertise and Medical Team-Ultrasound Test Team
La Jolla Vein & Vascular Expertise and Medical Team-Ultrasound Test Team




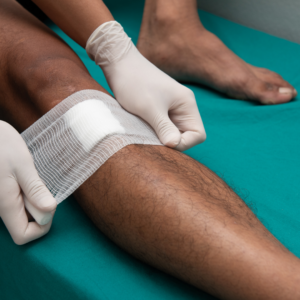
Non-healing ulcers, a condition more serious than typical wounds, can significantly affect your health. Unlike ordinary cuts, these ulcers require specialized attention and care. At La Jolla Vein & Vascular, we are committed to addressing non-healing ulcers and the complications they can cause. […]
In the realm of vascular health, chronic venous insufficiency (CVI) stands as a prevalent yet often misunderstood condition including leg ulcers. Characterized by a cascade of […]
Chronic Venous Insufficiency (CVI) presents itself as a medical condition stemming from untreated venous reflux disease, heralding a plethora of discomforting symptoms. If disregarded, it has the potential to give rise to substantial skin alterations and complications. In this blog post, we embark on a journey to decipher the essence of CVI, […]
Varicose veins, those twisted and bulging veins beneath the skin’s surface, affect countless individuals, often causing discomfort and concern. In this informative blog post, we’ll delve into the intricacies of varicose veins and the underlying venous reflux disease. From understanding the […]
As San Diego’s #1 top provider of varicose vein and vascular care, La Jolla Vein & Vascular is thrilled to announce being selected to be vein specialist providers for patients with Kaiser Permanente several months ago. Our physicians have passed rigorous credentialing by Kaiser Permanente and we now accept patients with Kaiser insurance. Please call […]
Revolutionizing Vascular Health with ClosureFast™: Endovenous Radiofrequency Ablation (RFA)In the realm of minimally invasive procedures, groundbreaking solutions like ClosureFast™ are reshaping the landscape. In this article, we embark on a journey to uncover the intricacies of ClosureFast™, an endovenous radiofrequency ablation […]
Varicose veins, those twisted and bulging veins visible beneath the skin’s surface, can cause significant concern for many individuals. While predominantly appearing in the legs, they can manifest in other parts of the body as well. This article delves into the realm of […]
Venous reflux disease, also known as venous stasis, venous insufficiency, or venous incompetence, is a multifaceted condition that affects the veins in the legs. In this article, we’ll take an in-depth look at venous reflux disease, including its underlying causes and the symptoms it presents. […]
Spider veins are the fine, thread-like reddish veins at the surface of the skin. These veins are not healthy. Veins are often considered a cosmetic issue, but they can be associated with underlying feeder veins, not […]
Vein Care, Reimagined®

Expert medical care. Advanced, minimally invasive treatments.
All FDA-approved options. One personalized plan.
CONTACT INFORMATION
La Jolla/UTC
9850 Genesee Ave, Suite 410, La Jolla, CA 92037
Vista
906 Sycamore Ave, Suite 100, Vista, CA 92081
Use the search features below to find articles and insights for the diagnosis and treatment of vascular disease
Vein Care, Reimagined®

Expert medical care. Advanced, minimally invasive treatments.
All FDA-approved options. One personalized plan.
CONTACT INFORMATION
9850 Genesee Ave, Suite 410, La Jolla, CA 92037
906 Sycamore Ave, Suite 100, Vista, CA 92081
Use the search features below to find articles and insights for the diagnosis and treatment of vascular disease