Restless Leg Syndrome & Venous Insufficiency
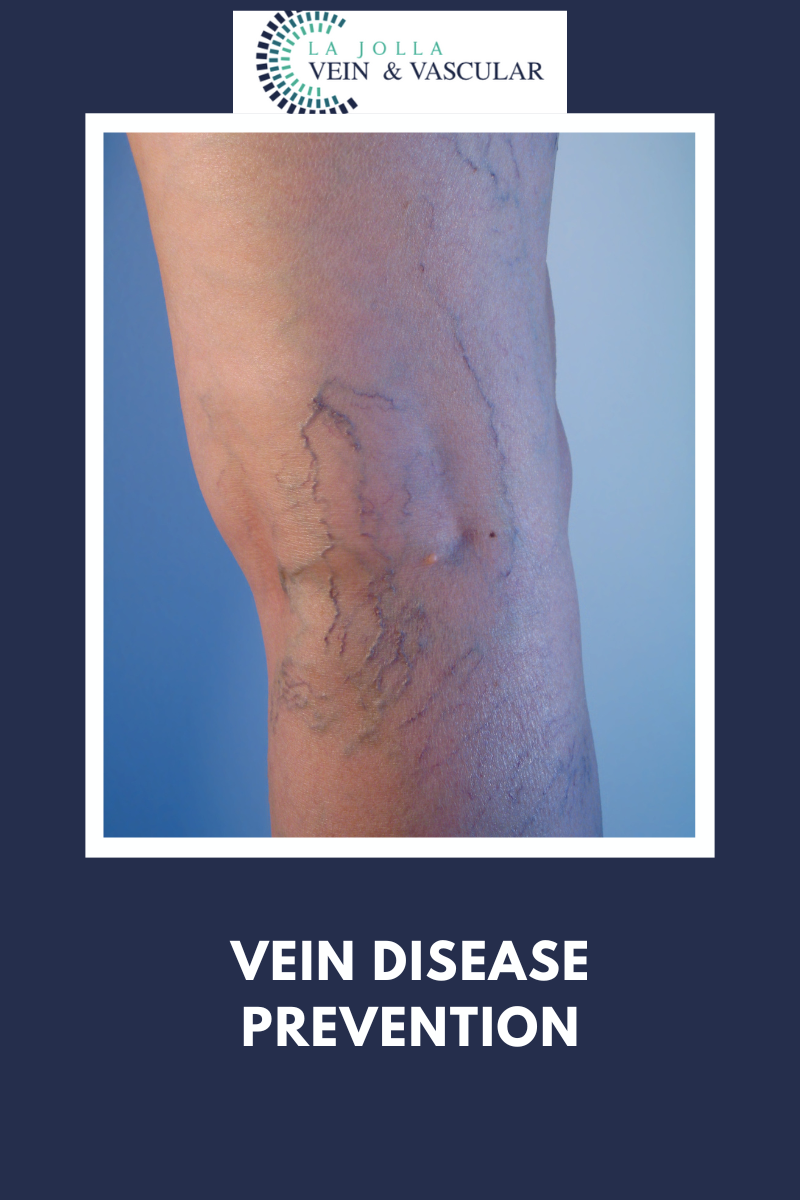
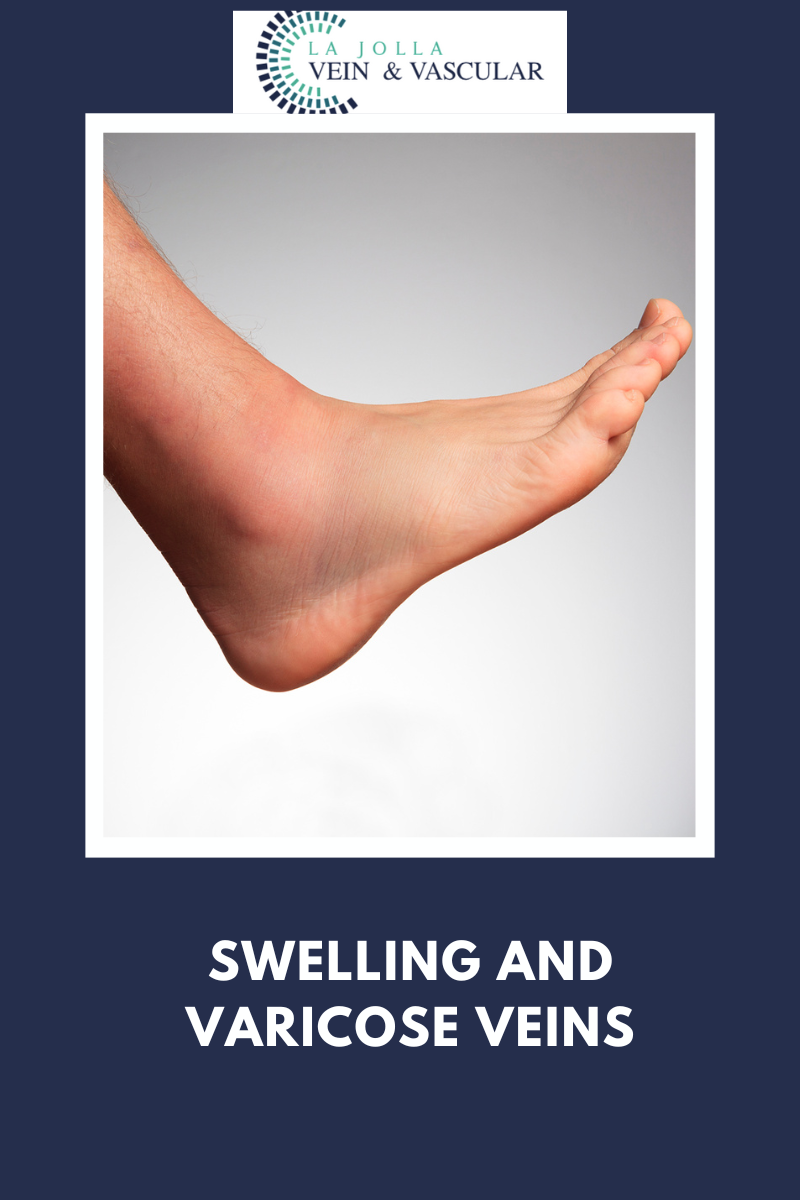
LJVascular2022-08-18T16:00:48-07:00Patients with varicose veins often report a feeling of restless legs, especially at night when in bed. In our study, about 30% of patients with varicose veins complained of restless legs.
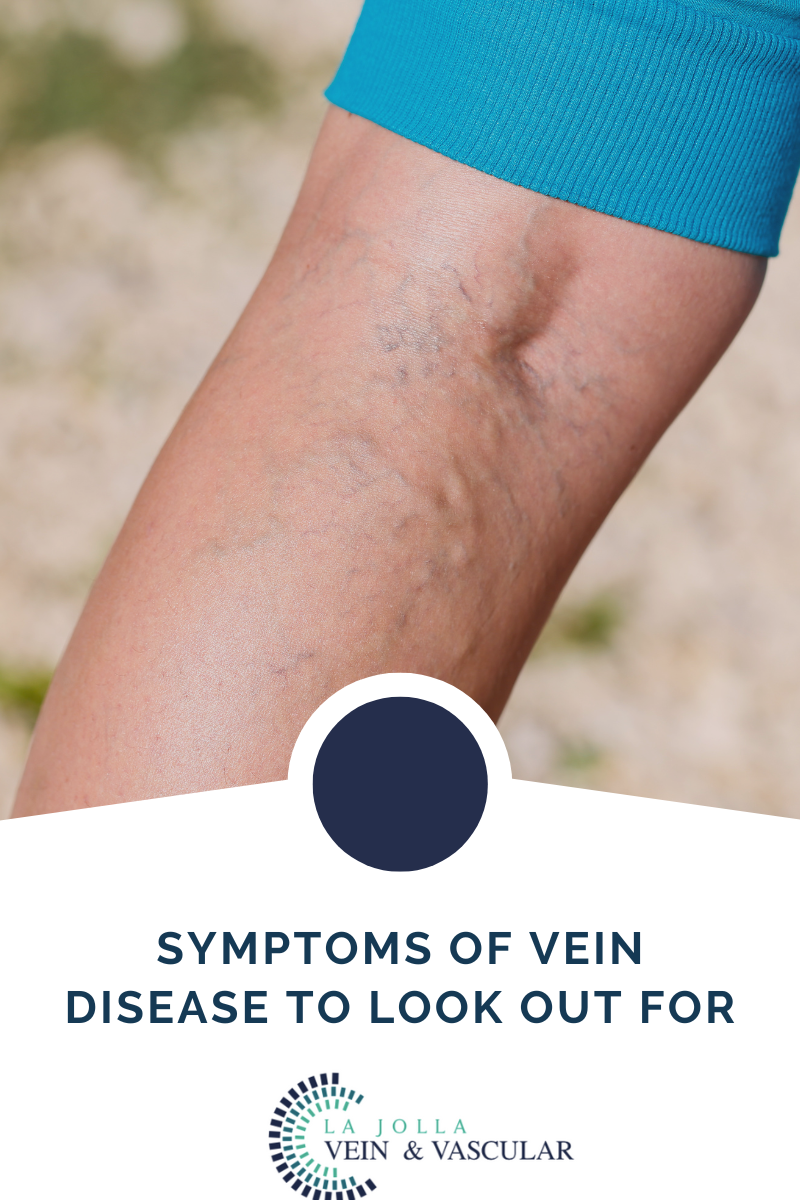
Restless legs syndrome (RLS) is a sensorimotor movement disorder characterized by uncomfortable sensations in the legs and an urge to move them. There are other causes of restless legs syndrome such as, neurological disorders, anemia, and kidney disease to name a few and are often treated with medication. Venous insufficiency is often neglected as a cause of Restless Legs Syndrome. However, when recognized, it is easily treatable leading to resolution of symptoms.
Treatment is aimed at correcting the underlying venous insufficiency. This usually is accomplished by removing the varicose veins or incompetent veins by new, minimally invasive, non-surgical methods. In our study, 98% of the patients with venous insufficiency and restless legs, had resolution of symptoms following treatment.
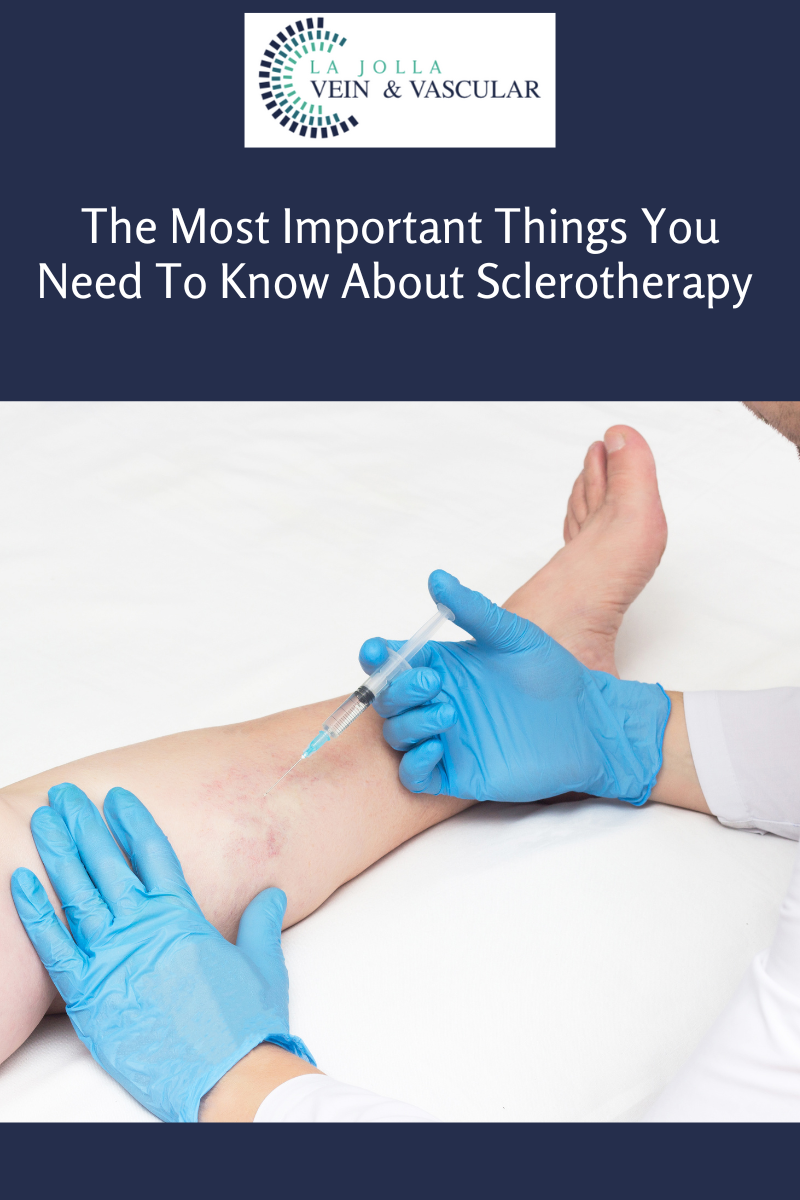
In another study, by Hayes, CL et. al, 35 patients with RLS and superficial venous insufficiency underwent endovenous ablation of refluxing superficial veins and ultrasound-guided sclerotherapy of varicose veins. 89% of patients reported alleviation of symptoms.
If a patient has restless legs symptoms and evidence of varicose veins of the legs, a work-up for venous insufficiency should be considered. The work-up involves a duplex ultrasound evaluation of the leg veins. This may eliminate the need for medication for RLS.
“Bringing Experts Together for Unparalleled Vein and Vascular Care”
La Jolla Vein & Vascular (formerly La Jolla Vein Care) is committed to bringing experts together for unparalleled vein and vascular care.
Nisha Bunke, MD, Sarah Lucas, MD, and Elliot DeYoung, MD are specialists who combine their experience and expertise to offer world-class vascular care.
Our accredited center is also a nationally known teaching site and center of excellence.
For more information and to book a consultation, please give our office a call at 858-550-0330.
For more information please check out our Youtube Channel at this link.
For more information on varicose veins and eliminating underlying venous insufficiency, check this link out full of resources.