Treatment for reticular veins
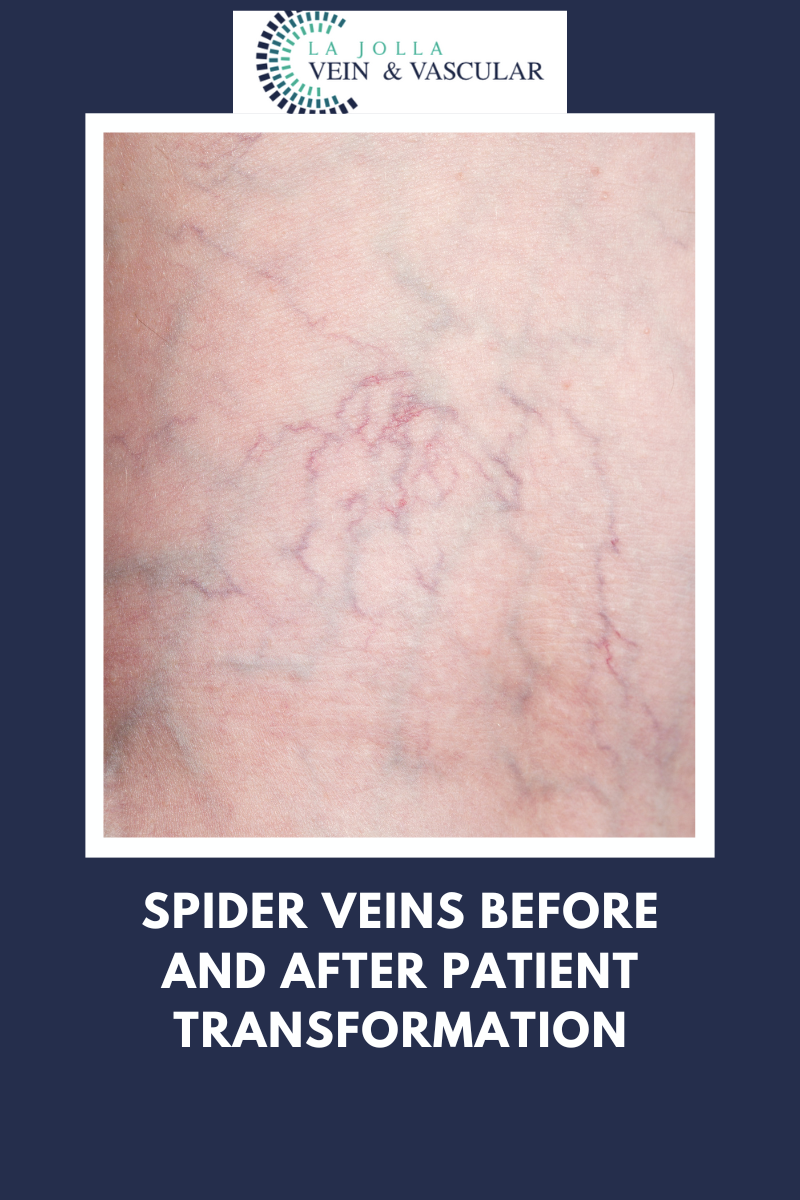
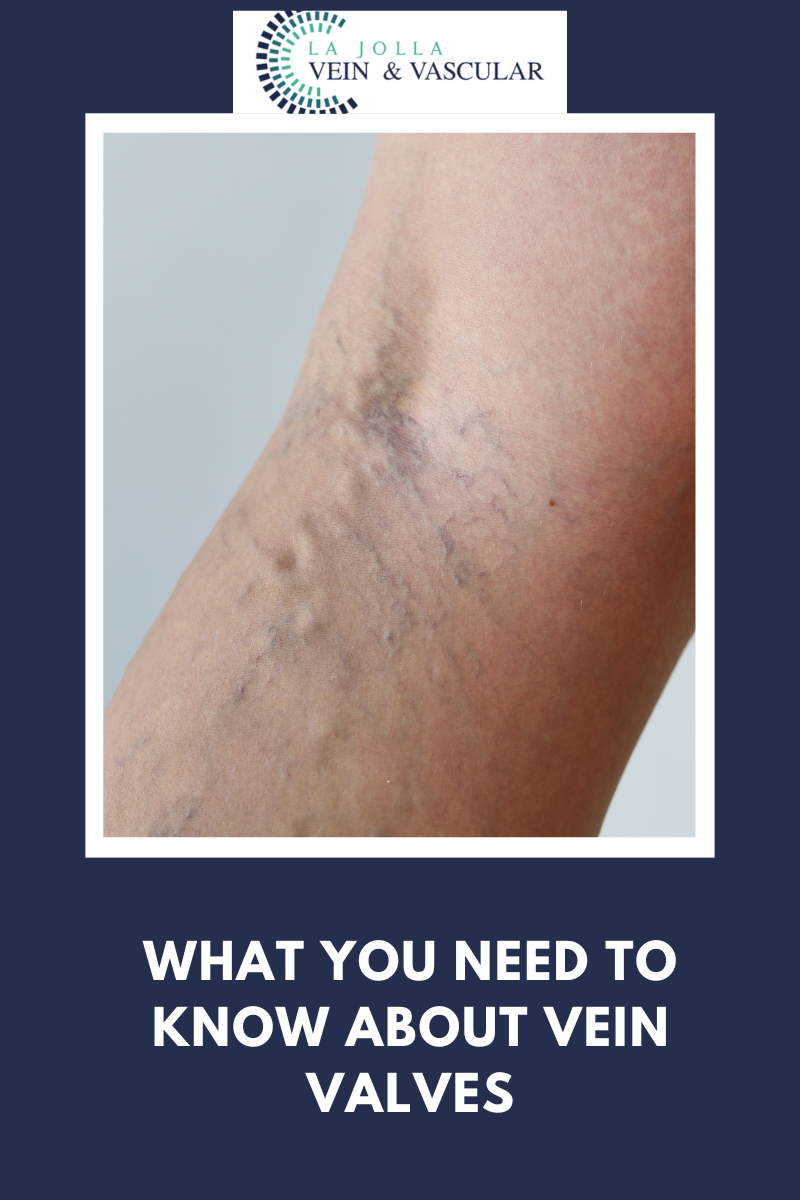
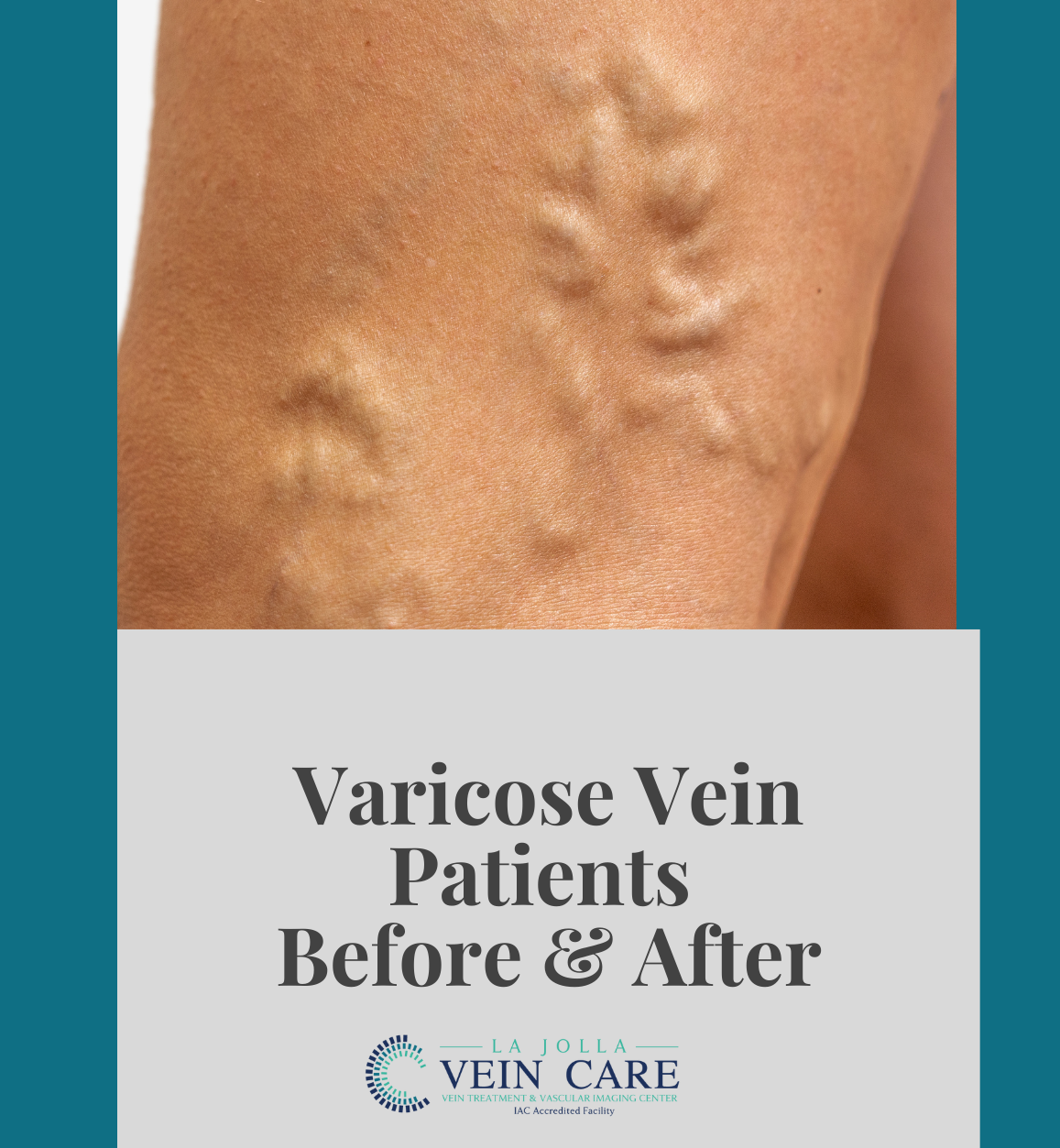
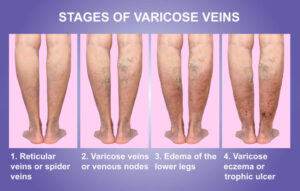
LJVascular2022-10-24T11:12:10-07:00The best treatment for Reticular Veins is through a painless alternative to traditional sclerotherapy: Cryo-Sclerotherapy.
Why have I been offered cryo-sclerotherapy?
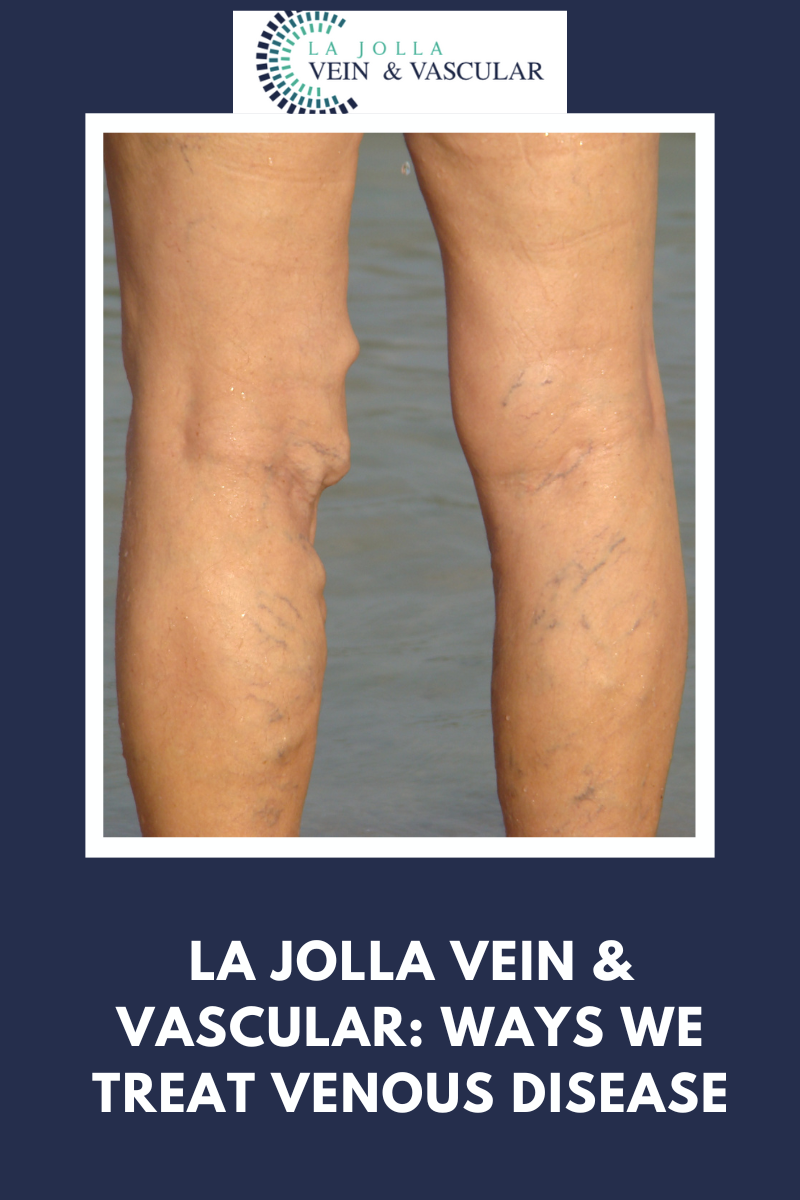
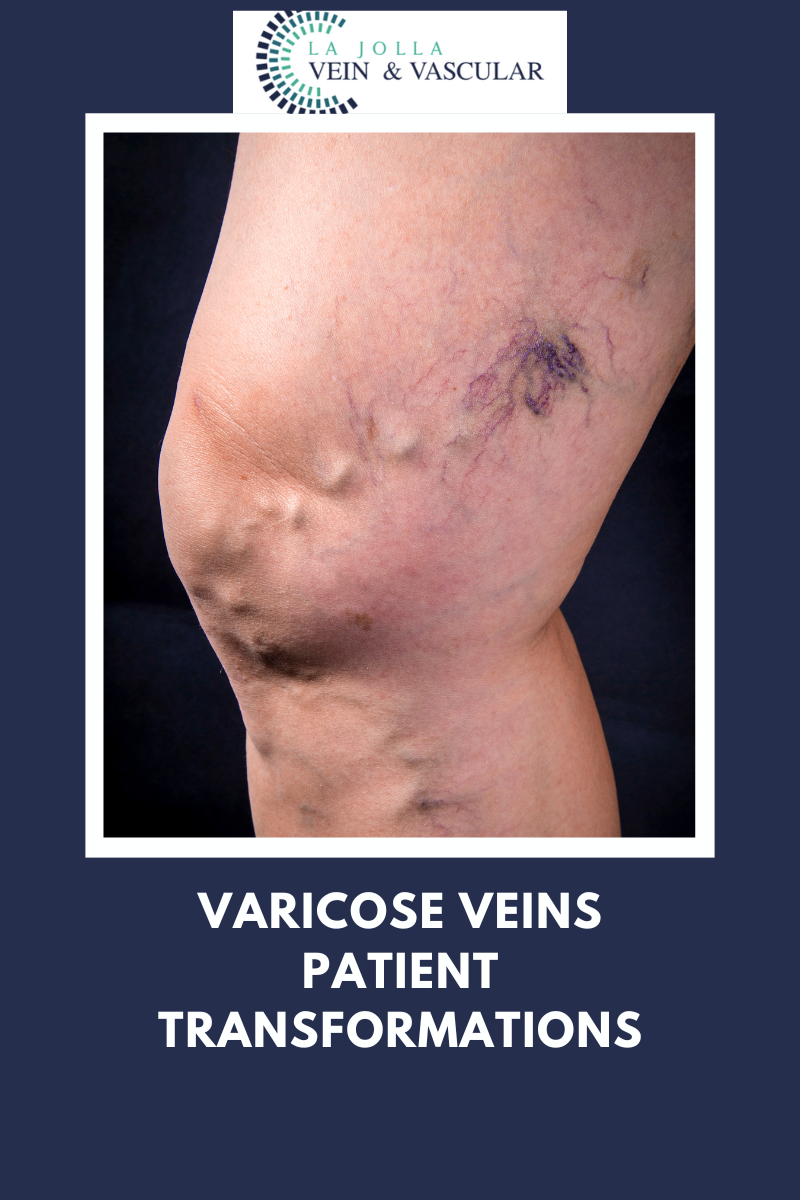
We recommend patients undergo cry-sclerotherapy to mainly treat spider veins and small varicose veins at the skin surface (also known as reticular veins). Traditional sclerotherapy involves injection of a medication into the […]