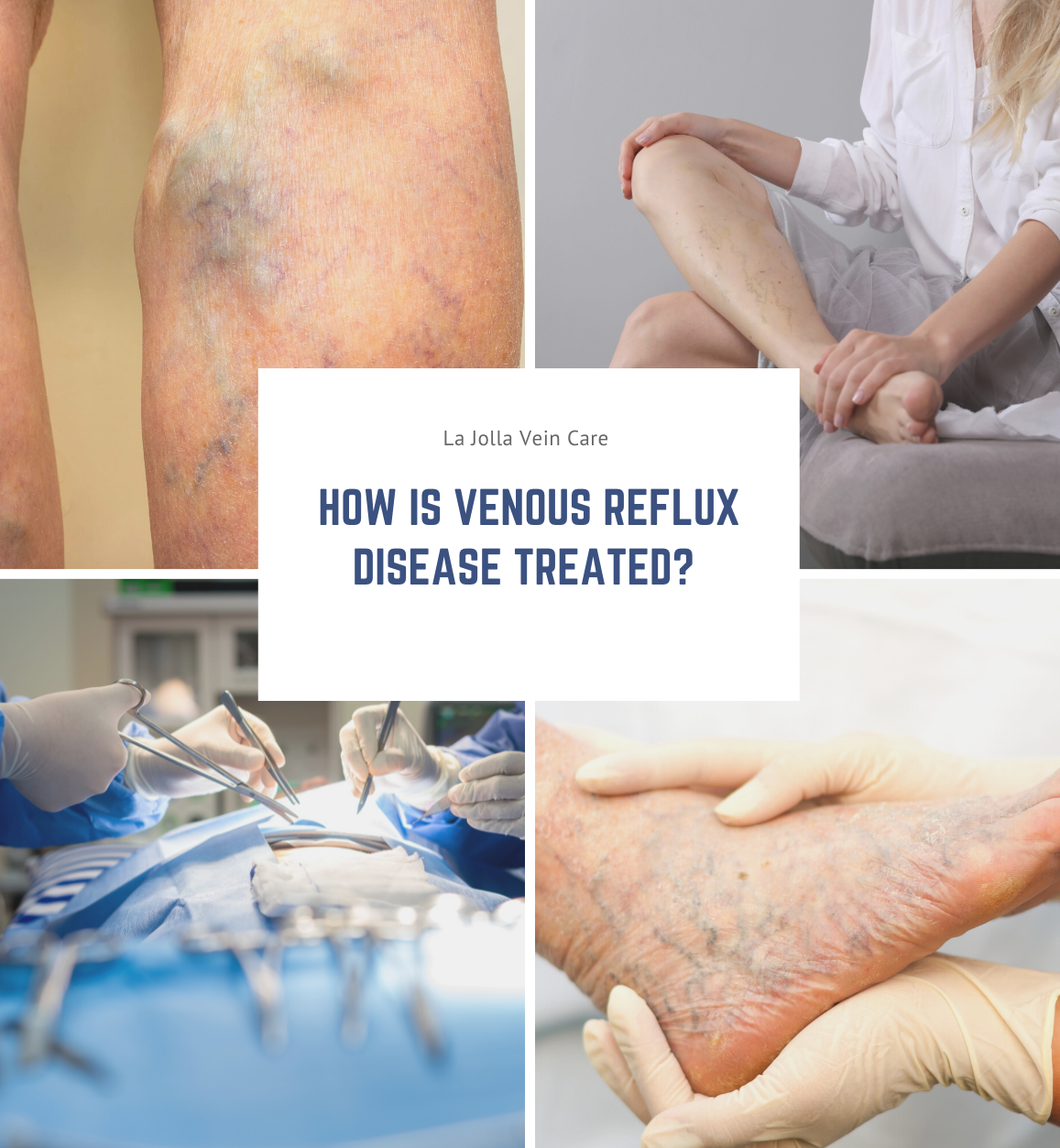
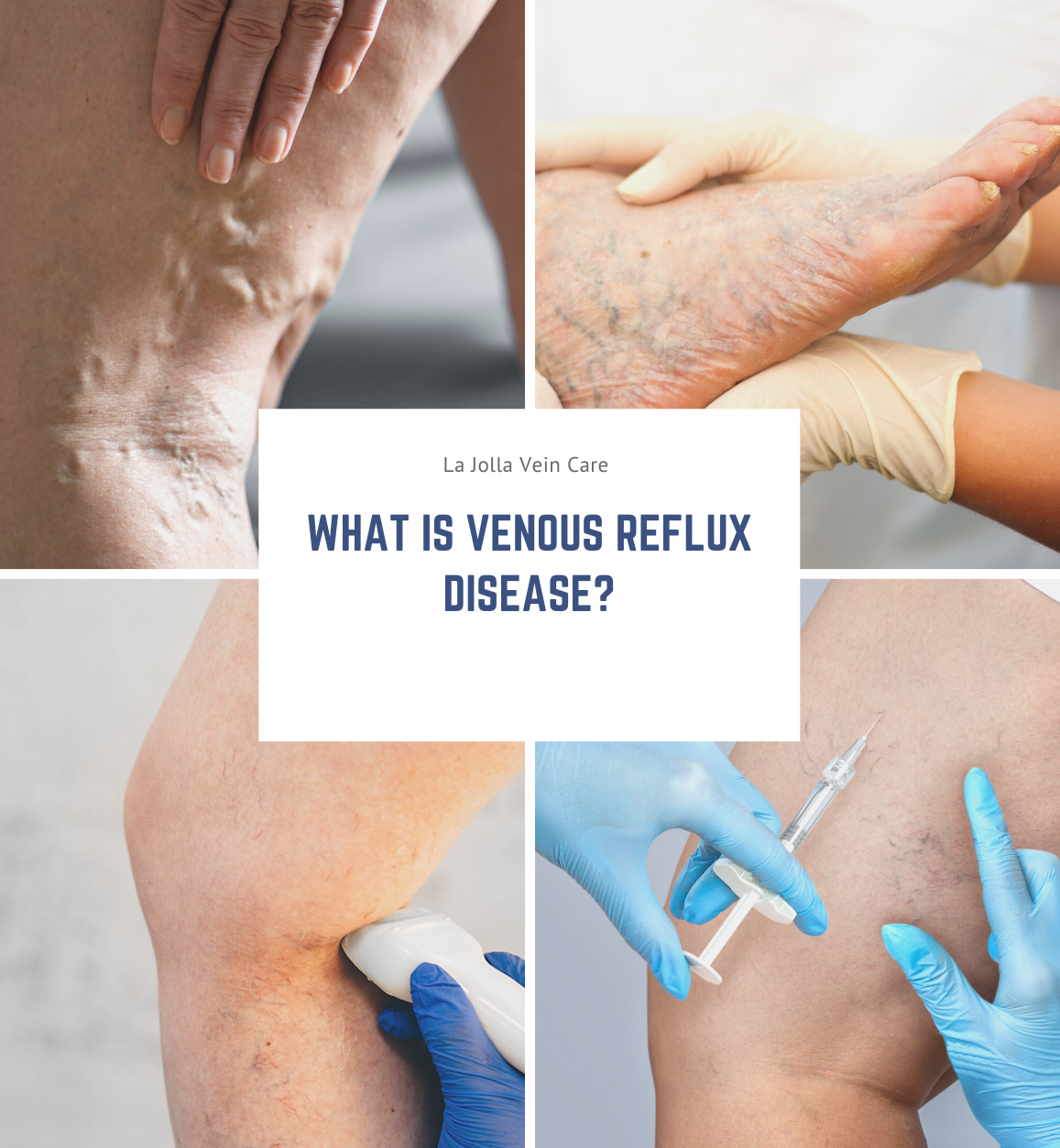
How is Venous Reflux Disease Treated?
LJVascular2022-03-17T10:19:57-07:00How is Venous Reflux Disease Treated?
Step 1: Identifying the underlying problem
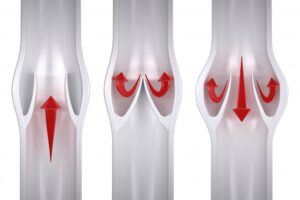
The first step is to treat the underlying problem, venous reflux disease. The specific pattern of venous reflux disease was detected by ultrasound. Venous reflux usually starts in the saphenous veins. The saphenous veins are most effectively treated with vein ablation procedures. This […]