Patient Reviews & Testimonials
LJVascular2023-02-15T15:40:22-08:00La Jolla Vein & Vascular is a state-of-the-art medical center dedicated exclusively to the diagnosis and treatment of vein and arterial conditions for patients.
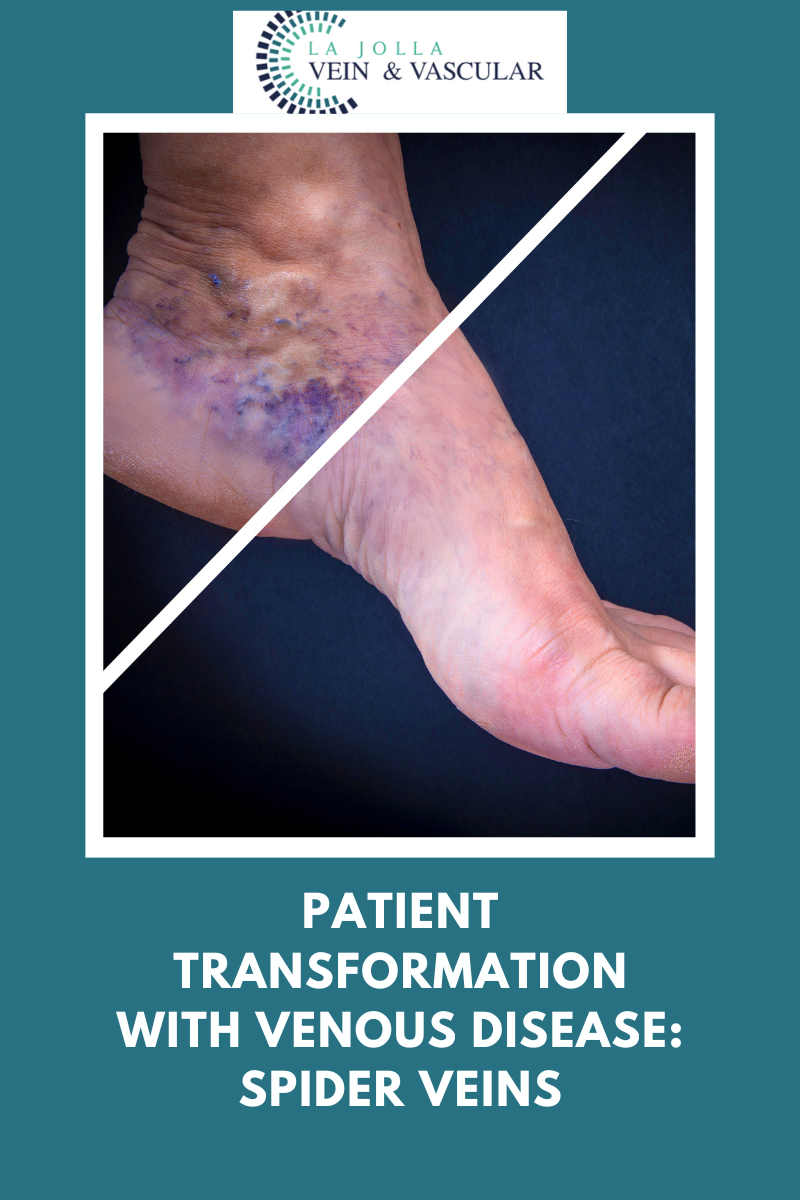
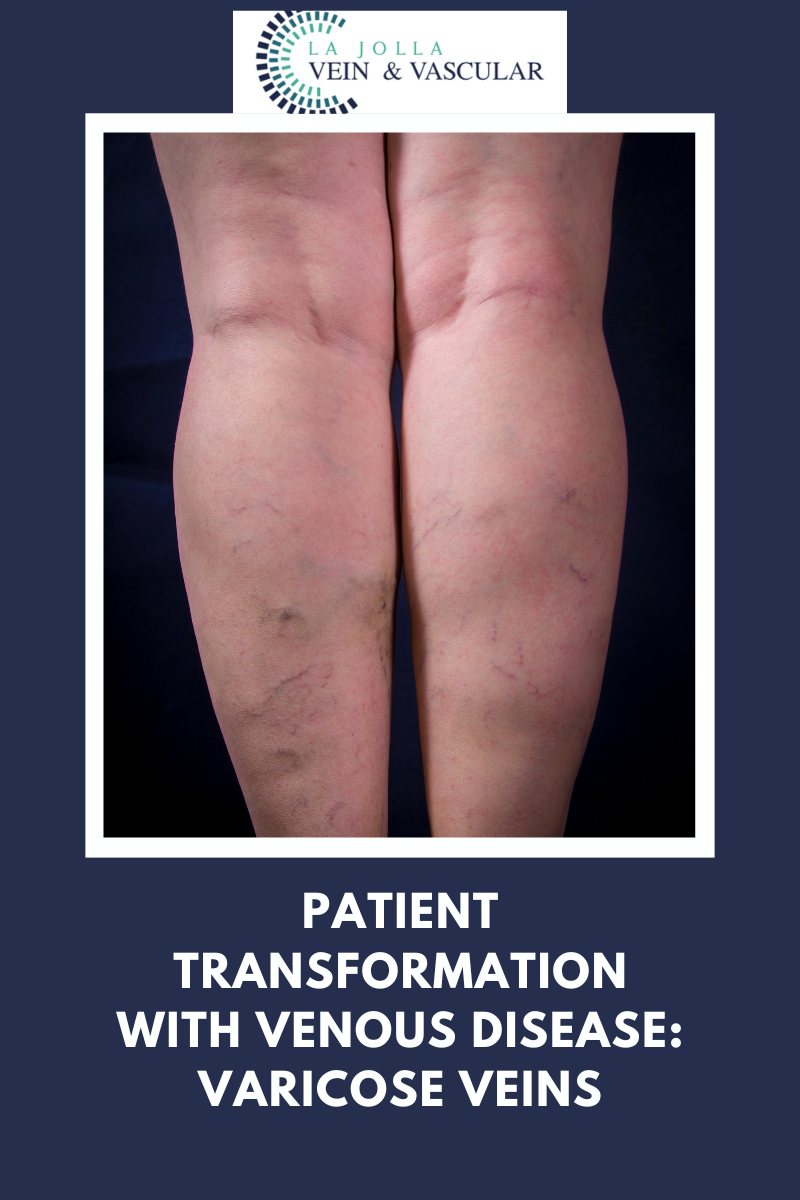
Vein conditions of patients we have treated include varicose veins, spider veins, and venous leg ulcers, chronic venous insufficiency, edema, lymphedema, and deep vein thrombosis. Arterial conditions and […]