Why have I been offered an endovenous laser ablation (EVLA) procedure?
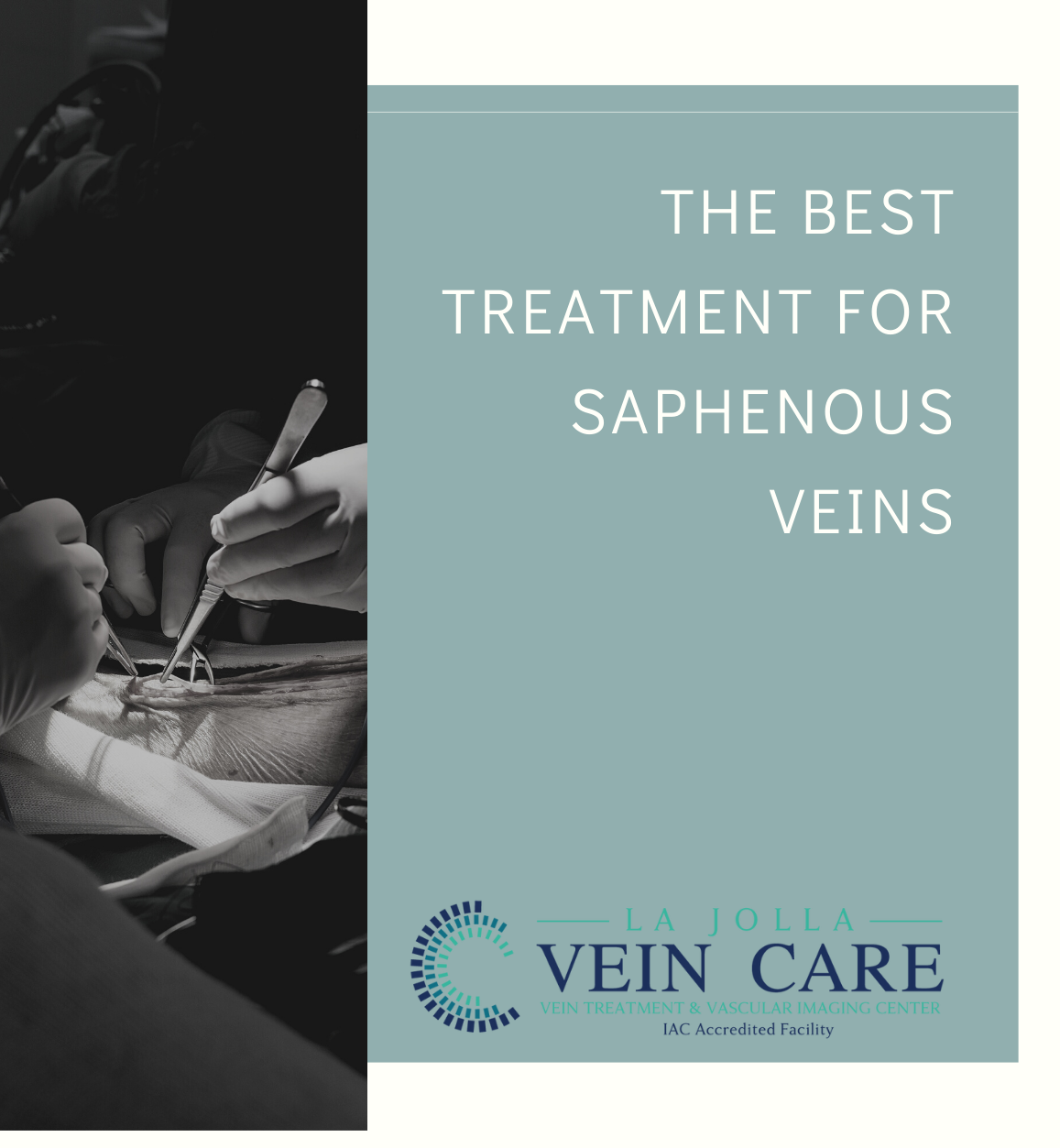
LJVascular2025-10-15T22:40:55-07:00Endovenous Laser Ablation for Saphenous Vein Reflux
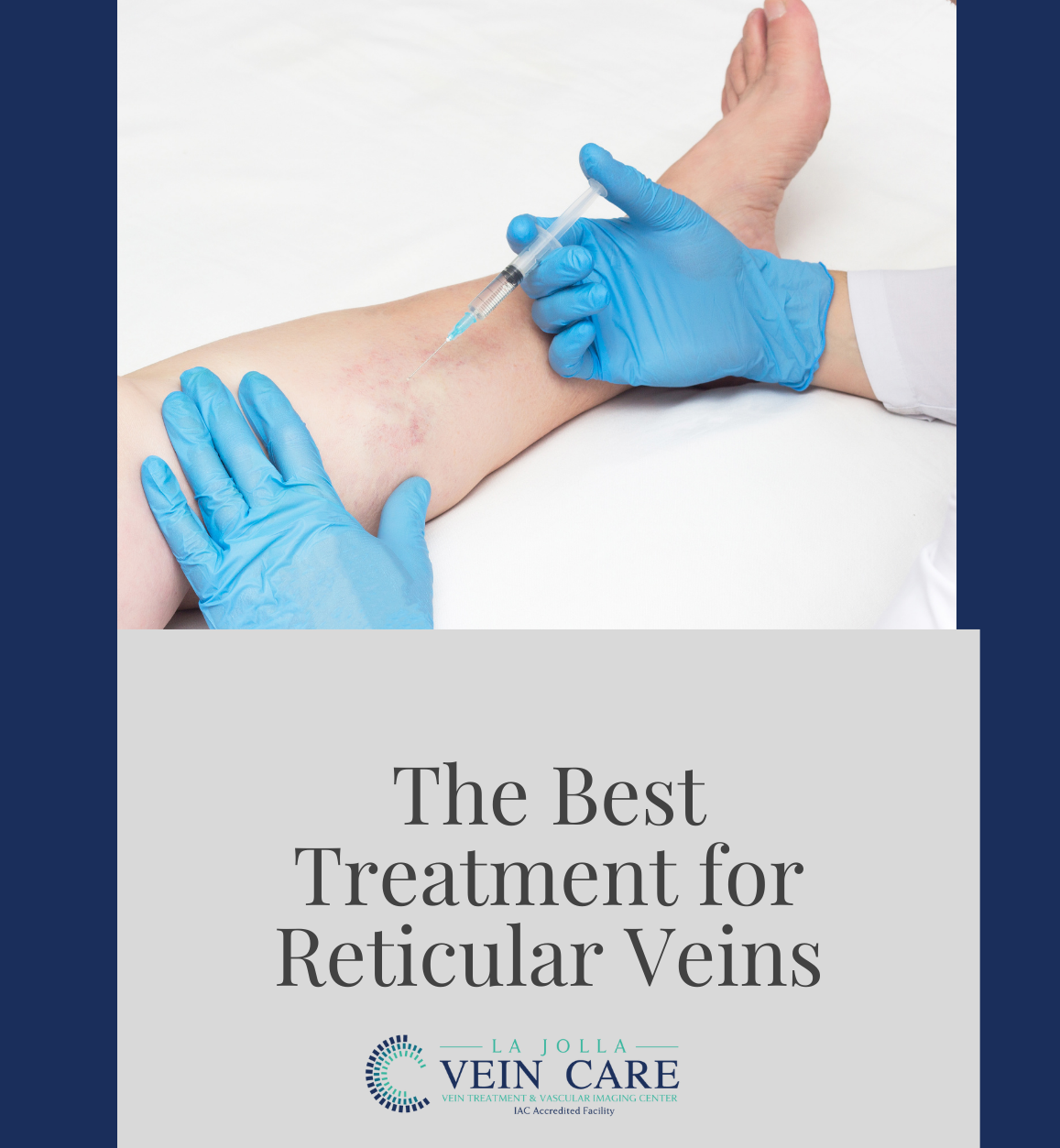
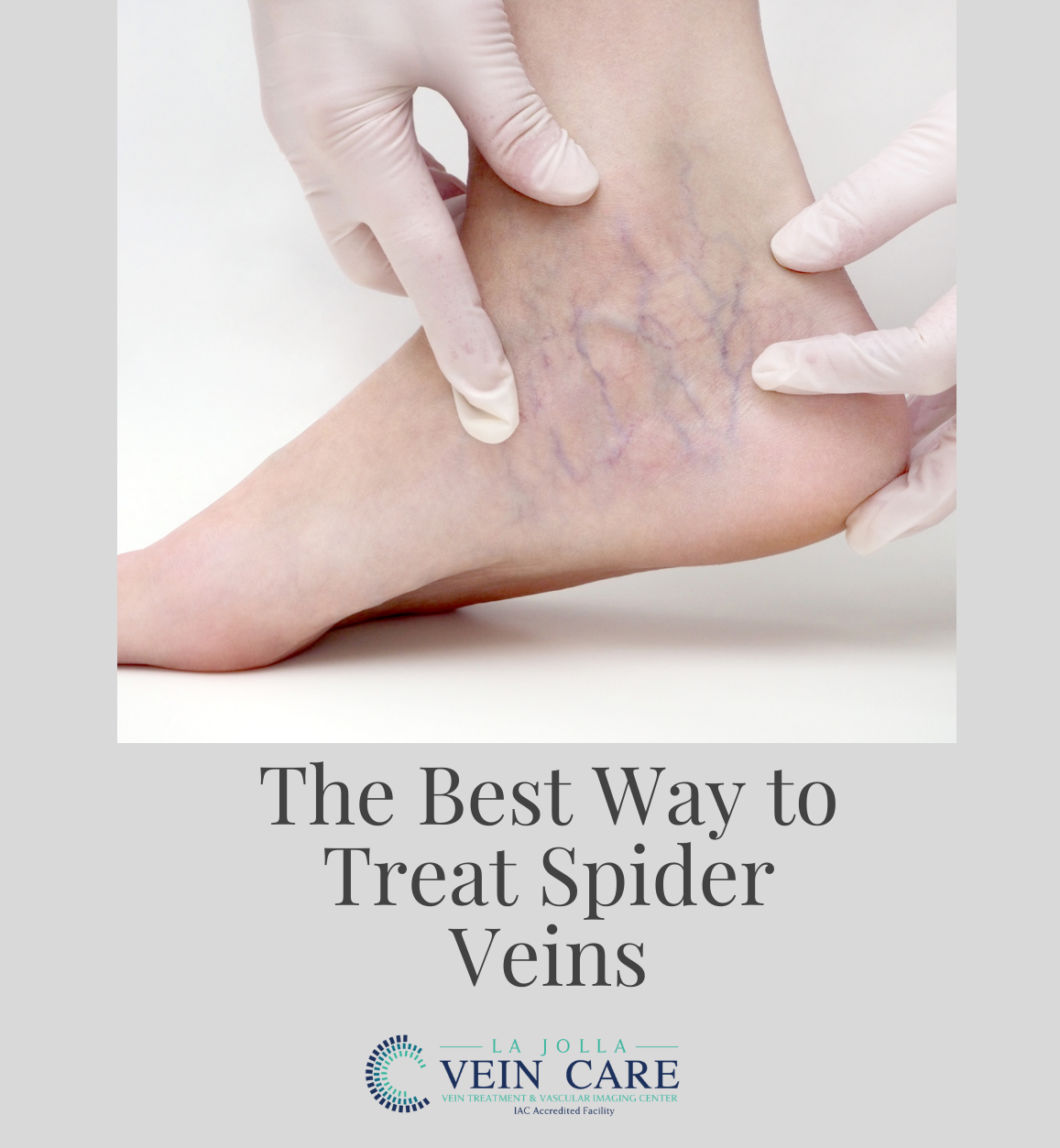
Endovenous laser vein ablation, also known as endovenous laser therapy (EVLA), is a type of treatment for saphenous vein reflux, the underlying cause of most varicose veins. At La Jolla Vein Care, we offer ALL treatment modalities for varicose veins, not just […]