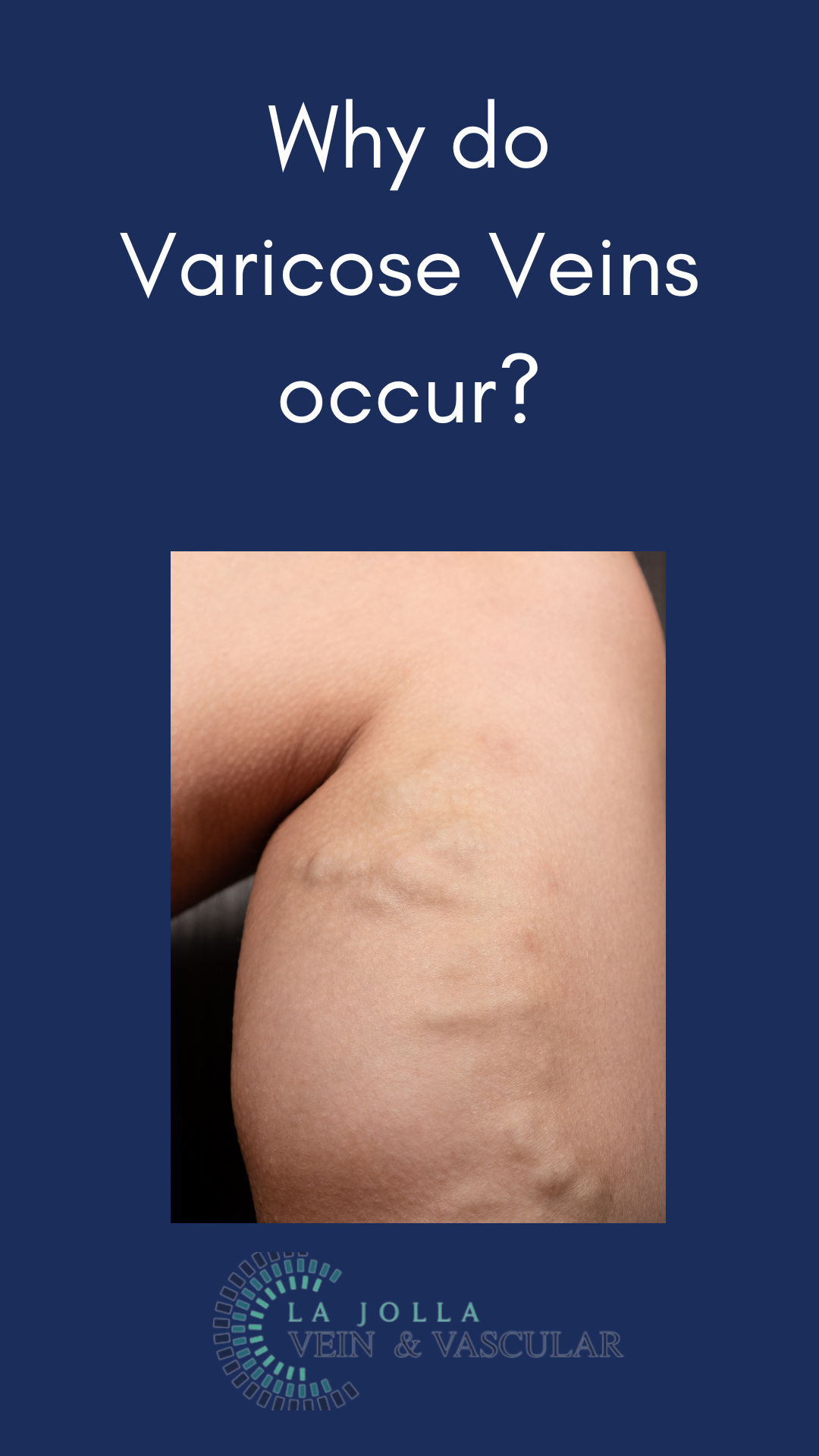
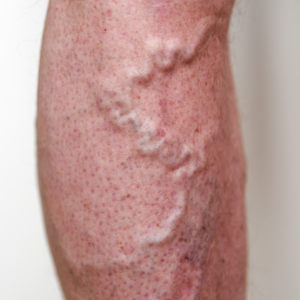
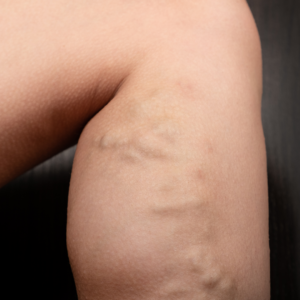
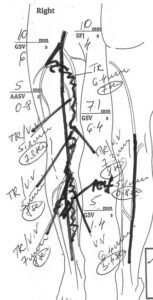
Why do Varicose Veins occur?
LJVascular2024-07-06T16:37:07-07:00Unveiling Key Insights: Your Comprehensive Guide to Understanding Varicose Veins
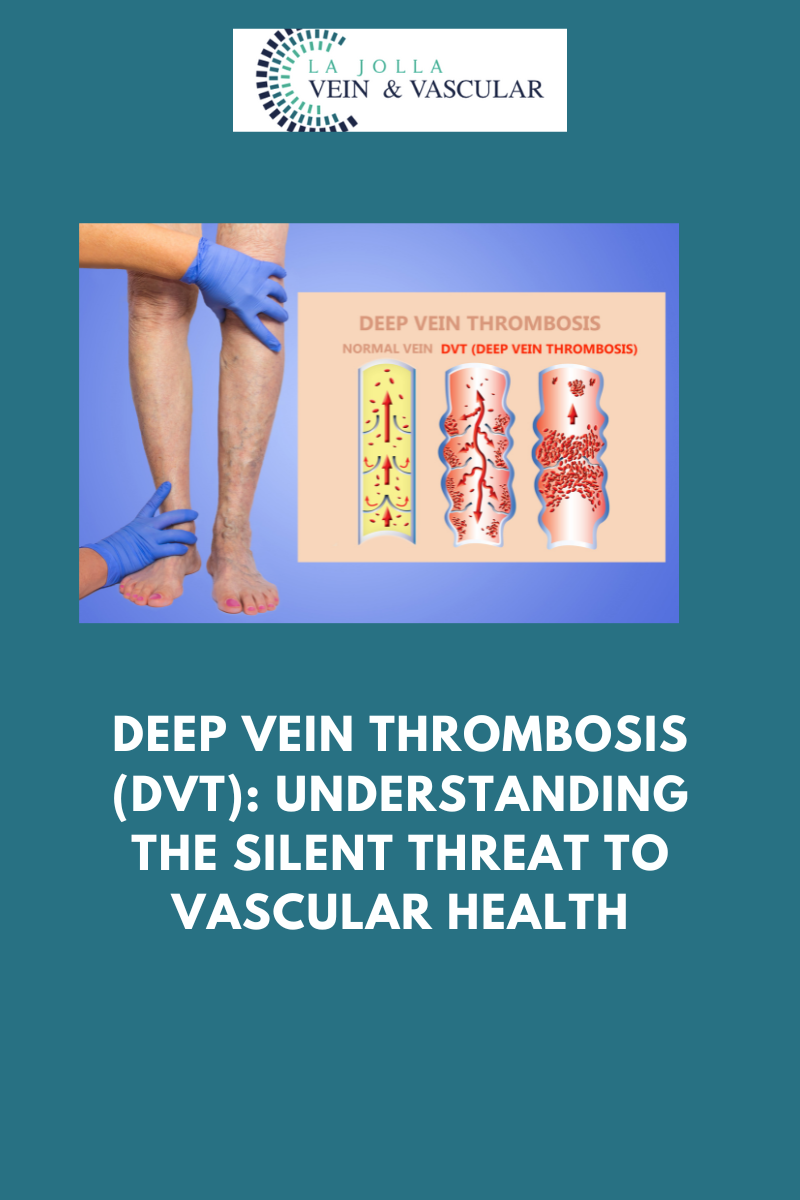
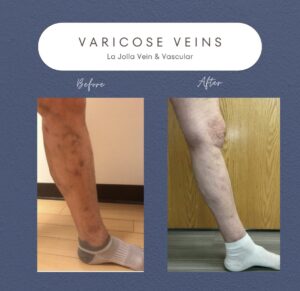
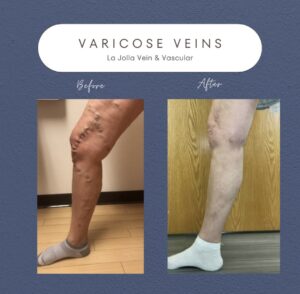
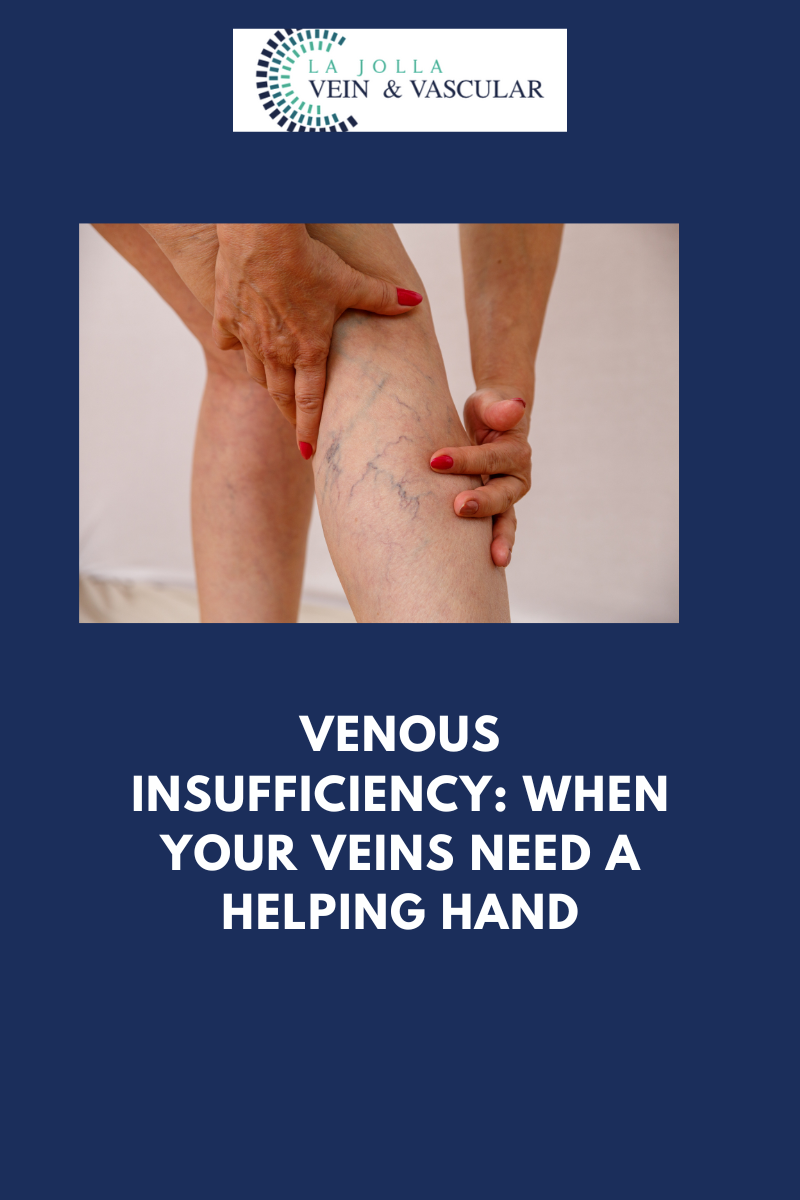
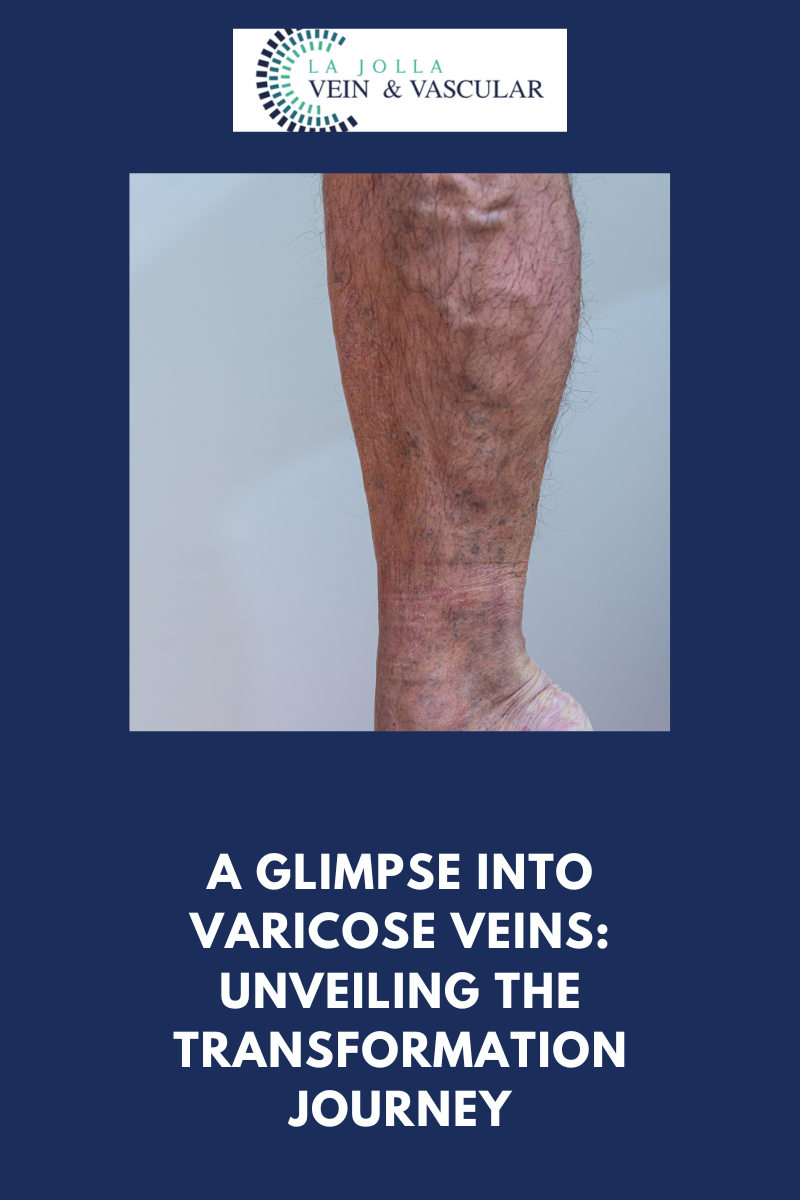
Varicose veins, those twisted and bulging veins beneath the skin’s surface, affect numerous individuals, often causing discomfort and aesthetic worries. This informative blog post aims to explore the intricacies of varicose veins and the underlying venous reflux disease. From comprehending the causes […]