Asclera: A New Treatment For Spider Veins and Small Varicose Veins
LJVascular2025-10-15T22:39:41-07:00What is polidocanol (Asclera)?
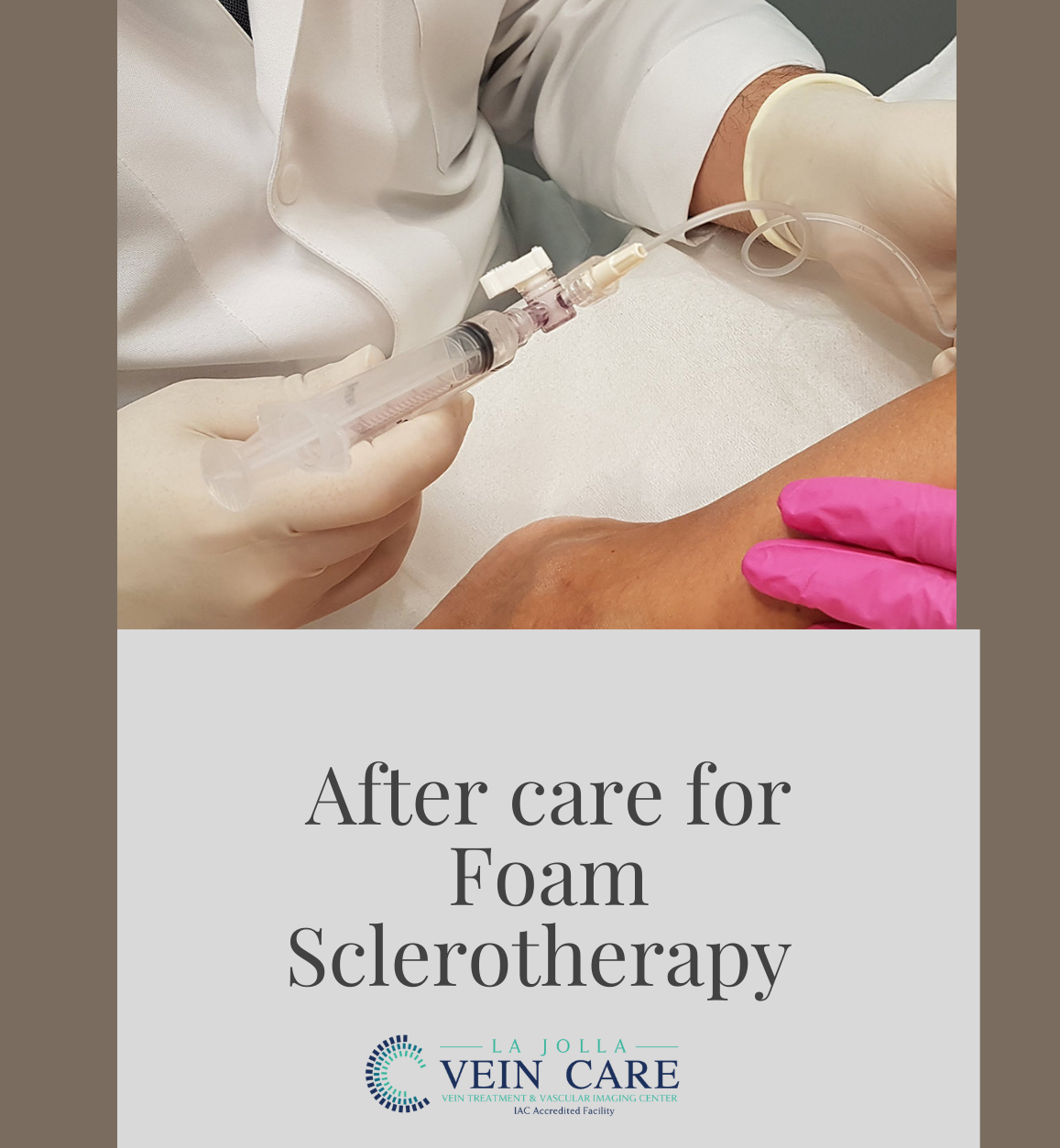
A variety of sclerosant medications can be used for veins, but at La Jolla Vein Care, we prefer polidocanol (brand name Asclera), because it is the most comfortable for the patient and has the lowest risk of side effects. It is a detergent-type medication that injures the inner lining of the veins. […]