What you need to know about DVT
What do Serena Williams, Richard Nixon, Dan Quayle, Dick Cheney and David Bloom have in common? They have all suffered a potentially fatal deep venous thrombosis (DVT).
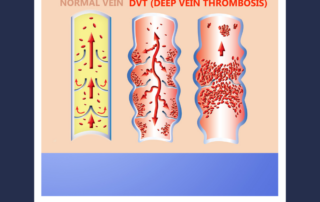
Deep venous thrombosis (DVT) mainly affects the large veins in the lower leg and thigh. The clot can block blood flow and cause swelling and […]