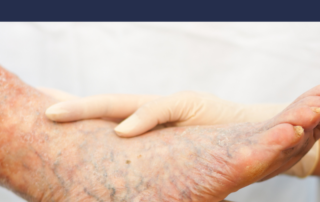
Muscle Hernia or Varicose Veins
Is it a muscle hernia or varicose vein?
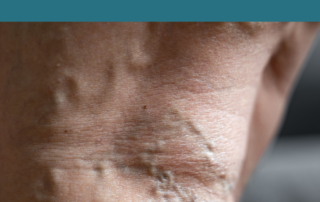
Muscle hernias of the legs frequently are confused with varicose veins. Patients may present with bulging along the outer part of the shin, that looks like a varicose vein. It may or may not be painful. It goes away with flexing the foot […]