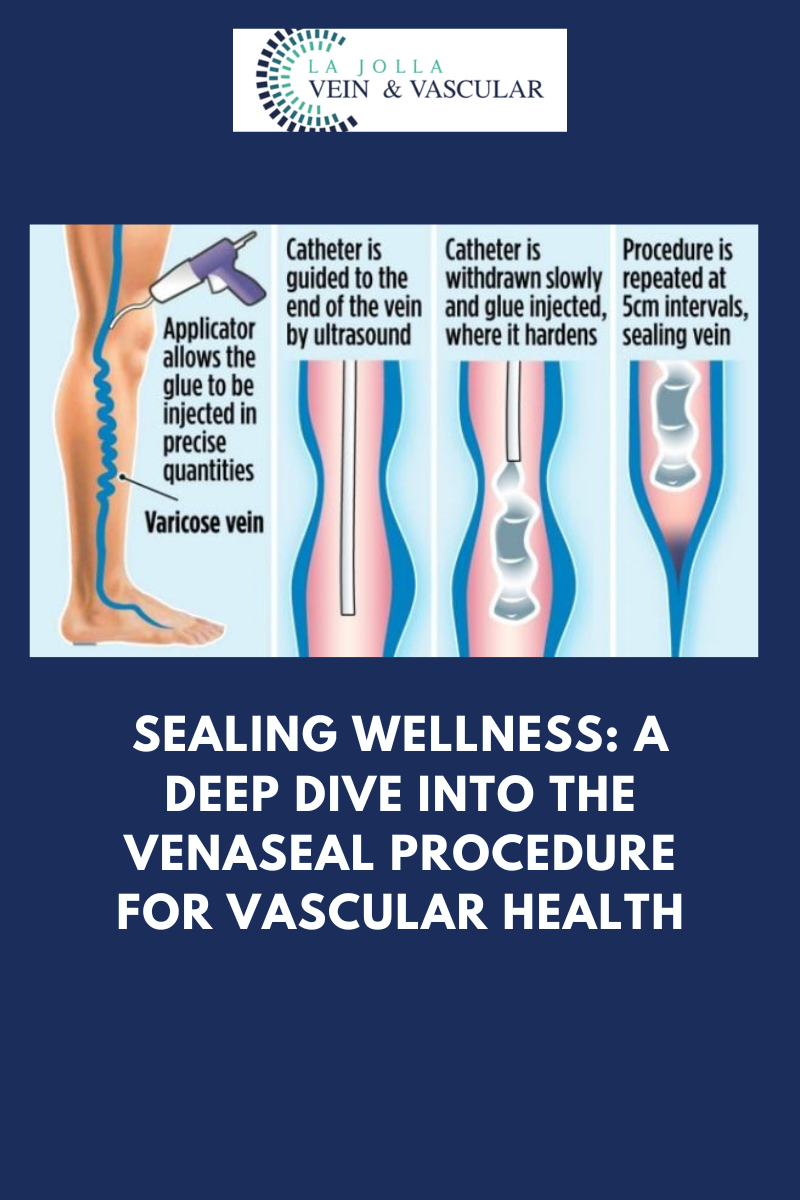
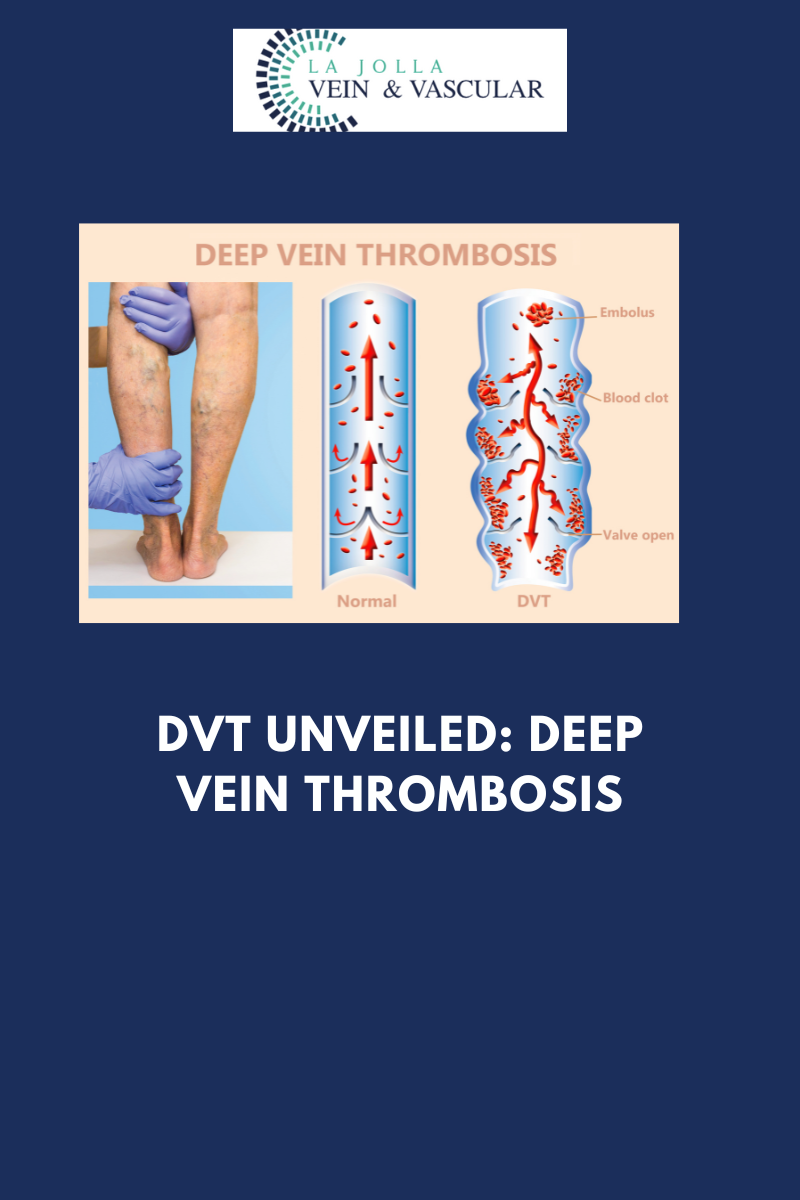
May Thurner Syndrome

Have you had a blood clot in the left leg, or recurrent blood clots without a known cause? Do you notice swelling of the left leg? If so, you may be considered for evaluation of May-Thurner Syndrome, which can be a hidden cause for left leg swelling and DVTs. May-Thurner Syndrome is a condition where the right common iliac artery overlies and compresses the left common iliac vein against the lumbar spine. This causes narrowing of the vein in the pelvic region, sort of like a bottle-neck. The narrowing of the vein makes the blood flow more sluggish and prone to blood clots and leg swelling. This variant has been shown to be present in over 20% of the population.
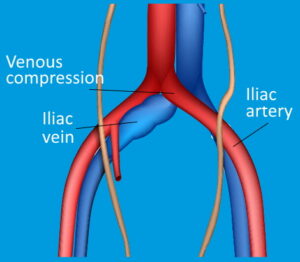
What Is May-Thurner Syndrome?
The iliac arteries originate from the largest artery in the body, the abdominal aorta. They split at the spine to form the left and right iliac arteries, which feed blood to the pelvis and legs. The right iliac artery is supposed to lie over the left iliac vein, but with this syndrome this artery is compressing the vein. As a result of this compression, the iliac vein narrows and constricts, sometimes scarring. This narrowing results in increased risk of developing blood clots or deep vein thrombosis in that extremity.
Why Do I Have May-Thurner Syndrome?
This condition is congenital but not hereditary and is more common in women than men. It shows up more frequently in young women taking birth control medication, as women age or as they gain weight. Many people may be unaware that they have this disorder, because many may only have some degree of compression of the iliac vein. Only a small number of individuals have severe compression of the iliac vein, resulting in symptoms, namely blood clots in the deep veins of the leg.
How Is May-Thurner Diagnosed?
Diagnosis is achieved by a combination of physical examination and diagnostic testing. Diagnosis may also occur when patients present with symptoms of a deep vein thrombosis (DVT- please see this section of venous conditions) and further testing is completed.
Tests to confirm diagnosis include:
- Duplex ultrasound
- Computed tomography scan (CT)
- Intravascular ultrasound
- Angiography
What Are My Treatment Options for May-Thurner Syndrome?
The goal of treatment is to reduce symptoms as well as reduce the risk of further complications.
- Anticoagulant therapy: These medications thin your blood and prevent the current clot from increasing in size, as well as prevent new clots from forming. These medications do not dissolve the clots that you have. You may be on IV heparin for several days or an injection called Lovenox that is given in the abdomen once daily for 5 to 7 days. You will be started on a medication called warfarin (Coumadin), which is an anticoagulant pill. It can take about 3 days for this medication to have effect, so during that time you may be on both warfarin and heparin. You may be on this medication for up to 6 months, during which time routine blood tests are required to ensure your blood is at the appropriate thinness to prevent clots from forming.
- Catheter-directed Thrombolytic Therapy: During this procedure, a thin flexible tube called a catheter is inserted into a puncture in the skin and guided into the affected blood vessel of the lung. A thrombolytic drug is injected which dissolves the clot over a period of time. There is a much higher risk of bleeding as well as stroke with this therapy, compared to anticoagulants.
- Angioplasty and stenting: Once the clot has been removed from the vein, this procedure is performed to widen the compressed vein. A thin flexible tube called a catheter is inserted in a puncture over a vein in the leg. A small balloon at the tip of the catheter is inflated to stretch the iliac vein open, increasing blood flow to the leg. A small metal mesh tube called a stent is inserted through the catheter and guided to the ballooned area of the iliac vein. The stent will help hold the compressed area open and will remain in the vein permanently.
- Inferior Vena Cava (IVC) filter: During this procedure, a thin flexible tube called a catheter is inserted through a vein in your leg, arm, or neck. The vascular surgeon passes a small special metal filter through the catheter and places it in the inferior vena cava, which is a large vein in your abdomen that carries blood back to the lungs. This filter traps clots that break away from leg veins, preventing them from travelling to your lungs. This is done if the patient cannot tolerate anticoagulation therapy.
“Bringing Experts Together for Unparalleled Vein and Vascular Care”
La Jolla Vein & Vascular (formerly La Jolla Vein Care) is committed to bringing experts together for unparalleled vein and vascular care.
Nisha Bunke, MD, Sarah Lucas, MD, and Elliot DeYoung, MD are specialists who combine their experience and expertise to offer world-class vascular care.
Our accredited center is also a nationally known teaching site and center of excellence.
For more information on treatments and to book a consultation, please give our office a call at 858-550-0330.
For a deeper dive into vein and vascular care, please check out our Youtube Channel at this link.
For more information on varicose veins and eliminating underlying venous insufficiency, check this link out full of resources.
Please follow our social media Instagram Profile and Tik Tok Profile for more fun videos and educational information.